Sex Differences in JAK-STAT Signaling: Implications for Precision Therapy in Ulcerative Colitis
This review synthesizes current evidence on sex-based differences in JAK-STAT pathway activation within the context of Ulcerative Colitis (UC).
Sex Differences in JAK-STAT Signaling: Implications for Precision Therapy in Ulcerative Colitis
Abstract
This review synthesizes current evidence on sex-based differences in JAK-STAT pathway activation within the context of Ulcerative Colitis (UC). We explore the foundational biology of sex hormones and genetic regulation on JAK-STAT signaling, detail methodologies for sex-stratified analysis in preclinical and clinical research, address challenges in experimental design and data interpretation, and evaluate comparative efficacy of JAK inhibitors across male and female patients. Targeting researchers and drug developers, this article aims to provide a roadmap for incorporating sex as a critical biological variable in the development of targeted immunotherapies for UC, ultimately guiding more personalized and effective treatment strategies.
The Biological Basis: How Sex Chromosomes and Hormones Modulate JAK-STAT in UC Pathogenesis
Thesis Context: JAK-STAT in Ulcerative Colitis Male vs. Female Research
Ulcerative colitis (UC), a chronic inflammatory bowel disease, exhibits sex-based disparities in prevalence, severity, and treatment response. The central thesis framing this guide is that differential JAK-STAT pathway activation and regulation between male and female patients may underpin these clinical variations, influencing the efficacy and targeting of emerging therapies.
Core Pathway Mechanics: A Stepwise Guide
The JAK-STAT pathway is the primary signaling mechanism for numerous cytokines implicated in UC immunopathology (e.g., IL-6, IL-12, IL-23, IFN-γ).
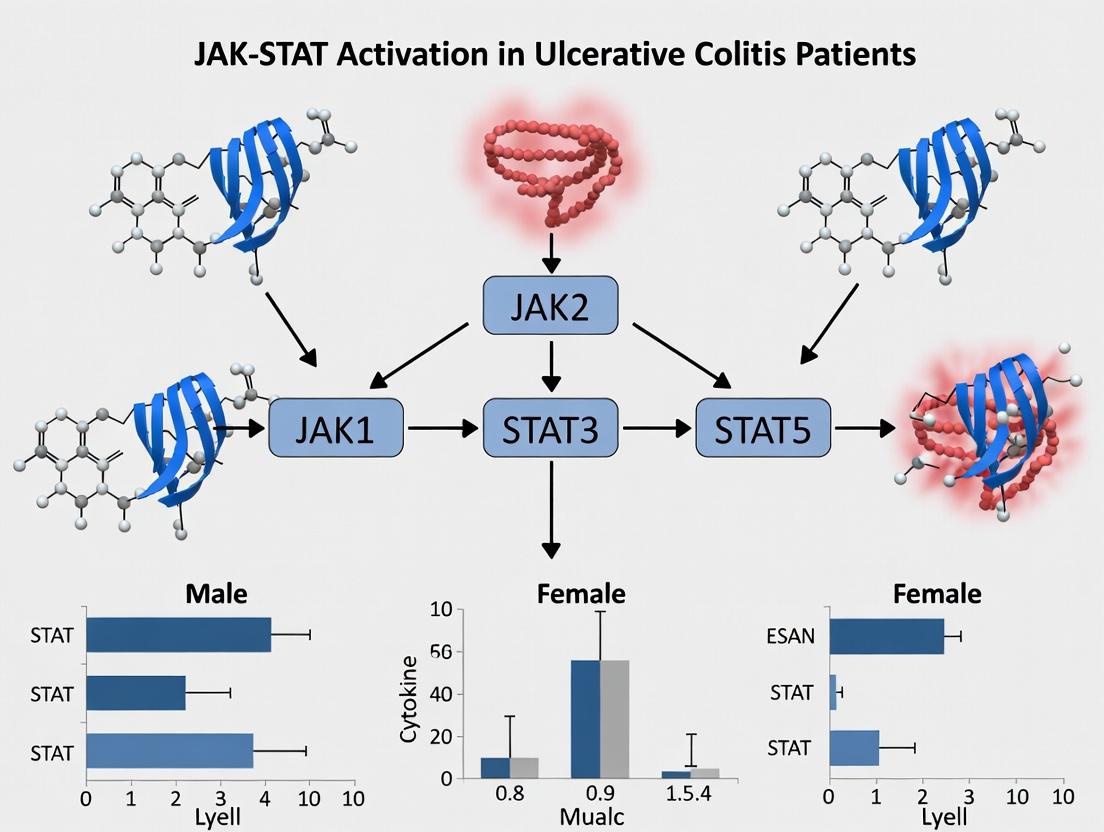
1. Cytokine Binding: A cytokine binds to its specific transmembrane receptor, inducing dimerization. 2. JAK Activation: Receptor-associated Janus Kinases (JAK1, JAK2, JAK3, TYK2) trans-phosphorylate each other. 3. Receptor Phosphorylation: Active JAKs phosphorylate tyrosine residues on the receptor cytoplasmic tails, creating docking sites. 4. STAT Recruitment & Phosphorylation: Cytosolic Signal Transducers and Activators of Transcription (STATs, e.g., STAT1, STAT3, STAT4) bind via their SH2 domains and are phosphorylated by JAKs. 5. STAT Dimerization & Nuclear Translocation: Phosphorylated STATs dimerize, translocate to the nucleus, and bind specific DNA sequences. 6. Gene Transcription: This binding regulates the transcription of target genes involved in inflammation, cell proliferation, and survival.
Comparison Guide: JAK Inhibitors in UC Clinical Development
The following table compares the performance of key JAK inhibitors based on published Phase 3 clinical trial data (induction and maintenance) in moderate-to-severe UC. Efficacy is measured by clinical remission, a composite endpoint.
Table 1: Efficacy Comparison of JAK Inhibitors in UC Phase 3 Trials
| JAK Inhibitor (Brand) | JAK Selectivity Profile | Induction Trial (Wk 8) Clinical Remission Rate | Maintenance Trial (Wk 52) Clinical Remission Rate | Key Safety Notes (from labels) |
|---|---|---|---|---|
| Tofacitinib (Xeljanz) | JAK1/JAK3 > JAK2 | OCTAVE 1: 18.5% (10mg BID) vs 8.2% (PBO) | OCTAVE Sustain: 41.3% (5mg BID) vs 11.1% (PBO) | Boxed Warning: Serious infections, malignancy, thrombosis, mortality. |
| Upadacitinib (Rinvoq) | JAK1 selective | U-ACHIEVE: 26.2% (45mg QD) vs 4.6% (PBO) | U-ACHIEVE Maint: 42.3% (15mg QD) vs 11.2% (PBO) | Boxed Warning: Serious infections, malignancy, thrombosis, mortality. |
| Filgotinib (Jyseleca) | JAK1 selective | SELECTION: 26.1% (200mg QD) vs 15.3% (PBO)* | SELECTION: 37.2% (200mg QD) vs 11.2% (PBO) | Warning: Serious infections, higher rates of herpes zoster. |
| Peficitinib (Not US/EU) | JAK3 preferential | PANTHER: 17.1% (75mg QD) vs 3.4% (PBO) | PANTHER: 27.9% (75mg QD) vs 7.0% (PBO) | Common AEs: Herpes zoster, increased blood creatinine. |
*In biologic-experienced patients. PBO = Placebo; BID = twice daily; QD = once daily.
Table 2: Experimental Data on Sex-Specific Efficacy Trends (Pooled Analysis)
| Parameter | Male Patients | Female Patients | Study Reference (Pooled) | Notes |
|---|---|---|---|---|
| Clinical Remission Rate (Upadacitinib 45mg) | ~30% | ~22% | Sands et al., Clin Gastroenterol Hepatol 2023 | Trend observed in induction data; requires further prospective study. |
| Serious Infection Rate (Tofacitinib) | 2.8 events/100 PY | 4.1 events/100 PY | Xeljanz US PI | Higher observed rate in females across trials. |
| STAT3 Phosphorylation in LP MCs | Higher baseline | Lower baseline | Galiez et al., Gut 2021 (ex vivo) | Lamina propria mononuclear cells (LP MCs) from untreated patients. |
Key Experimental Protocols
Protocol 1: Measuring STAT Phosphorylation in Colonic Biopsies (ex vivo)
- Objective: Quantify active, phosphorylated STAT (pSTAT) levels in intestinal tissue from male vs. female UC patients.
- Methodology:
- Sample Collection: Obtain pinch biopsies from inflamed colonic mucosa during colonoscopy. Immediately place in RNAlater or flash-freeze in liquid N2.
- Protein Extraction: Homogenize tissue in RIPA buffer with protease and phosphatase inhibitors.
- Western Blotting: Separate proteins by SDS-PAGE, transfer to PVDF membrane. Probe with antibodies against pSTAT3 (Tyr705), total STAT3, and β-actin (loading control).
- Quantification: Use densitometry to calculate the pSTAT3/total STAT3 ratio for each sample. Compare between sex-stratified cohorts.
Protocol 2: JAK Inhibitor Potency Assay (Cell-Based)
- Objective: Compare the inhibitory concentration (IC50) of different JAK inhibitors on IL-6-induced STAT3 phosphorylation.
- Methodology:
- Cell Culture: Use human T-cell line (e.g., Jurkat) or peripheral blood mononuclear cells (PBMCs).
- Inhibitor Pre-treatment: Incubate cells with a dose range (e.g., 1 nM - 10 µM) of each JAK inhibitor for 1 hour.
- Stimulation: Stimulate cells with recombinant human IL-6 (50 ng/mL) for 15 minutes.
- Detection: Fix and permeabilize cells. Stain intracellularly with anti-pSTAT3 (Alexa Fluor 488 conjugate). Analyze by flow cytometry.
- Analysis: Plot mean fluorescence intensity (MFI) vs. inhibitor concentration. Calculate IC50 values using non-linear regression.
Pathway and Workflow Visualizations
Title: JAK-STAT Pathway & Inhibitor Action in UC
Title: Ex Vivo pSTAT Analysis Workflow
The Scientist's Toolkit: Key Research Reagent Solutions
Table 3: Essential Reagents for JAK-STAT UC Research
| Reagent / Material | Function / Application | Example Vendor(s) |
|---|---|---|
| Phospho-STAT Specific Antibodies | Detection of activated (phosphorylated) STAT proteins in WB, IHC, or flow cytometry. | Cell Signaling Technology, Abcam |
| Recombinant Human Cytokines (IL-6, IL-12, IL-23) | Stimulation of the JAK-STAT pathway in in vitro or ex vivo cellular assays. | PeproTech, R&D Systems |
| JAK Inhibitor Small Molecules | Pharmacologic tools for pathway inhibition (positive controls, mechanism studies). | Selleckchem, MedChemExpress |
| RIPA Lysis Buffer with Phosphatase Inhibitors | Extraction of total protein while preserving phosphorylation states from tissue/cells. | Thermo Fisher, MilliporeSigma |
| Multiplex Phosphoprotein Assay Kits (Luminex/MSD) | High-throughput, quantitative measurement of multiple pSTATs from minimal sample. | MilliporeSigma, Meso Scale Discovery |
| STAT Reporter Cell Lines | Luciferase-based functional assay for STAT-dependent transcriptional activity. | BPS Bioscience, Promega |
This comparison guide is framed within a thesis investigating differential JAK-STAT activation in male versus female patients with ulcerative colitis (UC). The immune system exhibits pronounced sexual dimorphism, driven by sex hormones (estrogens and androgens) and genetic factors (e.g., X-chromosome-encoded genes). This guide objectively compares the influence of these variables on immune responses relevant to UC pathogenesis and treatment, with a focus on JAK-STAT signaling pathways.
Comparative Analysis of Hormonal and Genetic Regulation in UC-Relevant Immune Responses
Table 1: Comparative Effects of Estrogen and Androgen on Immune Cell Function and JAK-STAT Signaling
| Immune Parameter | Effect of Estrogen (e.g., 17β-Estradiol) | Effect of Androgen (e.g., Dihydrotestosterone) | Experimental Model (Reference) |
|---|---|---|---|
| Macrophage Polarization | Promotes anti-inflammatory M2 phenotype (IL-10↑, ARG1↑). | Promotes pro-inflammatory M1 phenotype (TNF-α↑, IL-1β↑). | Primary mouse BMDMs stimulated with LPS/IFN-γ (M1) or IL-4 (M2) + hormone treatment. |
| T helper Cell Differentiation | Enhances Th2 responses (IL-4, IL-5↑); modulates Treg function via FoxP3. | Suppresses Th1/Th17 responses (IFN-γ, IL-17↓). | CD4+ T-cells from human PBMCs or mouse splenocytes differentiated under polarizing conditions. |
| JAK-STAT Pathway Activity | Activates STAT3 in dendritic cells; modulates STAT1/STAT5. | Suppresses JAK1-STAT1/STAT4 signaling in T-cells. | Luciferase reporter assays (STAT-binding elements) in hormone-treated immune cell lines. |
| Cytokine Profile in UC Context | Reduces IL-6, TNF-α production in colonic lamina propria. | Associated with elevated IL-23/IL-17 axis in male patients. | Ex vivo culture of human UC colon biopsies; hormone receptor antagonist studies. |
| Epithelial Barrier Function | Enhances wound healing and mucin production via ERβ. | Can increase intestinal permeability in stress models. | Transepithelial electrical resistance (TEER) measurement in Caco-2 cells with hormone treatment. |
Table 2: Impact of Genetic Sex (XX vs. XY) and X-Chromosome Genes on Immune Dysregulation
| Genetic Variable | Immune System Impact | Association with UC Susceptibility/Severity | Supporting Experimental Data |
|---|---|---|---|
| X-Chromosome Inactivation (XCI) Escape | Double dosage of immune-related genes (e.g., TLR7, CD40L) in XX immune cells. | Higher prevalence of autoimmunity; may correlate with female UC severity flares. | Allele-specific expression analysis in female immune cell subsets (CD4+ T-cells, B cells). |
| Y-Chromosome Genes (e.g., SRY) | Modulates catecholamine synthesis, affecting macrophage activation. | Potential link to male-specific risk loci and treatment response. | ChIP-seq for SRY binding in male THP-1 macrophage cells. |
| X-linked miRNA (e.g., miR-18, miR-106a) | Regulates TLR4 and STAT3 expression. | Differential serum levels correlate with sex-biased therapeutic outcomes to JAK inhibitors. | qPCR of miRNAs isolated from serum of male/female UC patients pre/post JAKi therapy. |
| Epigenetic Regulation | Differential DNA methylation on X-chromosome in CD8+ T-cells. | Methylation status of FOXP3 intron 1 affects Treg stability differently by sex. | Whole-genome bisulfite sequencing of FACS-sorted T-cells from UC patients. |
Experimental Protocols for Key Cited Studies
Protocol 1: Assessing Hormonal Modulation of JAK-STAT in Primary Human Monocyte-Derived Macrophages
Objective: To quantify the effect of 17β-estradiol (E2) vs. dihydrotestosterone (DHT) on STAT phosphorylation.
- Cell Isolation & Differentiation: Isolate CD14+ monocytes from healthy donor PBMCs (male/female) using magnetic beads. Differentiate in RPMI-1640 + 10% charcoal-stripped FBS + 50 ng/mL M-CSF for 6 days.
- Hormone Treatment: Pre-treat macrophages for 24h with: a) Vehicle control, b) 10 nM E2, c) 100 nM DHT, d) E2 + ER antagonist (ICI 182,780).
- Stimulation & Lysis: Stimulate cells with 20 ng/mL IFN-γ for 30 minutes. Lyse using RIPA buffer with phosphatase/protease inhibitors.
- Analysis: Perform Western blotting for p-STAT1 (Tyr701), total STAT1, and β-actin. Quantify band intensity via densitometry.
Protocol 2: Sex-Differentiated Gene Expression in UC Lamina Propria Lymphocytes
Objective: To profile X-linked gene escape and JAK-STAT pathway transcripts.
- Tissue Processing: Obtain endoscopic biopsies from UC patients (matched disease activity). Process lamina propria mononuclear cells (LPMCs) via collagenase/DNase digestion.
- Cell Sorting: Sort live CD3+CD4+ T-cells and CD19+ B-cells using FACS into male (XY) and female (XX) pools.
- RNA-seq Library Prep: Extract total RNA, prepare stranded libraries. Include UMIs for accurate quantification.
- Bioinformatic Analysis: Align to GRCh38. Use tools like XCI-escape atlas to identify escaped genes. Perform GSEA on JAK-STAT signaling pathway sets (MSigDB).
Visualizations
Title: Sex Hormone and Genetic Regulation of Immune Bias and JAK-STAT
Title: Workflow for Analyzing Sex-Specific JAK-STAT in UC
The Scientist's Toolkit: Key Research Reagent Solutions
| Reagent/Material | Supplier Examples | Function in SABV/UC Research |
|---|---|---|
| Charcoal-Stripped FBS | Gibco, Sigma-Aldrich | Removes endogenous steroids for controlled hormone studies in cell culture. |
| Recombinant Human/Mouse Sex Hormones (E2, DHT) | R&D Systems, Sigma-Aldrich | For precise dosing in vitro and in vivo models to mimic physiological/pathological levels. |
| Selective Hormone Receptor Antagonists (e.g., ICI 182,780, Flutamide) | Tocris, MedChemExpress | To confirm receptor-specific effects in mechanistic studies. |
| Phospho-STAT Specific Antibodies (Flow/WB) | Cell Signaling Technology, BD Biosciences | To quantify activation states of JAK-STAT pathways in sex-stratified samples. |
| JAK Inhibitors (e.g., Tofacitinib, Upadacitinib) | Selleck Chem, MedChemExpress | Positive controls for pathway inhibition; used in ex vivo patient tissue cultures. |
| Magnetic Cell Separation Kits (Human/Mouse) | Miltenyi Biotec, STEMCELL Tech | Isolation of specific immune cell populations (e.g., CD4+ T-cells, CD14+ monocytes) from mixed samples. |
| X-Chromosome Inactivation Escape Atlas | Public Database (e.g., UCSC Genome Browser) | Bioinformatic resource to identify escaped genes in RNA-seq data from female cells. |
| Single-Cell RNA-seq Kits (3’/5’ with UMIs) | 10x Genomics, Parse Biosciences | To profile sex differences in immune cell heterogeneity and pathway activity at single-cell resolution from UC biopsies. |
Clinical Evidence of Sex Disparities in UC Incidence, Severity, and Treatment Response
This comparison guide examines the clinical evidence for sex-based differences in ulcerative colitis (UC), framed within the broader thesis of differential JAK-STAT pathway activation between male and female patients. Understanding these disparities is critical for drug development and personalized treatment strategies.
Comparative Analysis of UC Epidemiology by Sex
Table 1: Sex Disparities in UC Incidence and Disease Course
| Parameter | Male Patients | Female Patients | Key Supporting Studies & Notes |
|---|---|---|---|
| Overall Incidence | Generally lower | Generally higher | Meta-analysis (Shah et al., 2021): Pooled IRR = 1.18 for females vs. males. |
| Age at Onset | Bimodal peak (20-30s, 50-60s) | Pronounced peak in reproductive years (20-30s) | Hormonal influences implicated in female incidence peak. |
| Disease Extent | More left-sided colitis | More extensive (pancolitis) | Cohort study (n=12,000): Females had 1.3x higher odds of extensive disease. |
| Disease Severity | Higher risk of severe acute flare hospitalization | Higher reported symptom burden and extraintestinal manifestations | PRO data indicates higher abdominal pain and fatigue in females. |
| Surgical Colectomy | Higher long-term risk | Lower long-term risk | Population study: 20-year cumulative risk: Males 15.4%, Females 9.8%. |
Comparison of Treatment Response by Sex
Table 2: Differential Response to UC Therapies by Biological Sex
| Therapeutic Class | Male Patient Response | Female Patient Response | Experimental/Clinical Evidence |
|---|---|---|---|
| Anti-TNFα (e.g., Infliximab) | Better clinical remission rates | Lower remission rates, higher immunogenicity | Post-hoc analysis of ACT trials: Week 8 remission, Males 45%, Females 33%. Higher anti-drug antibodies in females. |
| Vedolizumab (α4β7 Integrin) | Comparable efficacy | Comparable efficacy, potential PK differences | GEMINI 1 analysis: No significant efficacy difference by sex. Population PK models suggest lower drug clearance in females. |
| JAK Inhibitors (e.g., Tofacitinib) | Robust efficacy in induction & maintenance | Reduced efficacy signal in maintenance phase | OCTAVE post-hoc: Females had lower remission rates vs. males at 52 weeks (OR 0.5, p<0.05). |
| Ustekinumab (IL-12/23p40) | Strong response in induction | Strong response in induction | UNIFI trials: No significant sex-based efficacy differences reported. |
Experimental Data on JAK-STAT Activation in Male vs. Female UC
Table 3: Experimental Evidence for Sex-Biased JAK-STAT Signaling
| Experimental Readout | Findings in Male UC Models/Patients | Findings in Female UC Models/Patients | Protocol Summary |
|---|---|---|---|
| Colonic pSTAT3 Levels | Higher baseline and cytokine-induced phosphorylation. | Lower baseline activation, but greater dynamic range with estrogen. | Protocol: Colonic biopsy lysates from sex-stratified patients. Western blot for pSTAT3 (Tyr705). Stimulation with IL-6 (50ng/mL, 30 min). Densitometry normalized to total STAT3. |
| PBMC STAT1 Phosphorylation | Moderate IFN-γ induced response. | Exaggerated pSTAT1 response to IFN-γ. | Protocol: Isolated PBMCs, serum-starved, stimulated with IFN-γ (100 IU/mL, 20 min). Flow cytometry for pSTAT1. Gating on CD45+ leukocytes. |
| JAK Inhibitor Efficacy In Vivo | Marked reduction in disease activity index (DAI) and histology. | Attenuated DAI response; greater residual STAT1 activity. | Protocol: DSS colitis in C57BL/6 mice. Oral Tofacitinib (10 mg/kg BID). DAI scored daily. Colonic tissue analyzed for pSTAT1/3 via multiplex IHC. |
| Estrogen Receptor (ERβ) Modulation | Minimal effect of ERβ agonism on STAT3. | ERβ agonist (LY3201) significantly suppresses IL-6-pSTAT3 axis. | Protocol: Female colonic organoids treated with IL-6 ± ERβ agonist (100nM). qPCR for SOCS3 and Western for pSTAT3. |
The Scientist's Toolkit: Key Research Reagent Solutions
Table 4: Essential Reagents for Investigating Sex Disparities in JAK-STAT/UC
| Item | Function & Application in Sex-Disparity Research |
|---|---|
| Phospho-STAT Specific Antibodies (e.g., pSTAT3 Tyr705) | Detects activated JAK-STAT pathway components in tissue (IHC) or cell lysates (WB/Flow). Critical for comparing baseline signaling between sexes. |
| Sex-Hormone Receptor Modulators (ERβ agonists, AR antagonists) | To mechanistically dissect hormonal influence on immune cell signaling in vitro and in vivo. |
| Cytokine Stimulation Panels (IL-6, IL-23, IFN-γ) | Used on PBMCs or biopsies to probe for sex-specific immune cell responsiveness and STAT phosphorylation dynamics. |
| Sex-Specific Preclinical Models (Gonadectomized, hormone-replaced mice) | Allows isolation of chromosomal vs. hormonal contributions to disease phenotypes and treatment responses. |
| Multiplex Immunohistochemistry (GeoMx, Phenocycler) | Enables spatial profiling of JAK-STAT pathway activity within the mucosal immune landscape from male vs. female tissues. |
| JAK Inhibitor Compounds (Tofacitinib, Upadacitinib) | Positive control compounds for testing sex differences in pathway inhibition efficacy in cellular and animal models. |
Signaling Pathway and Experimental Workflow Diagrams
Diagram 1: Sex-Modulated JAK-STAT Signaling in UC
Diagram 2: Workflow for Testing Sex Differences in UC
Hypotheses Linking Sex Differences to Divergent JAK-STAT Activation States
Within the context of research on ulcerative colitis (UC), a chronic inflammatory bowel disease with documented sex disparities in incidence and potential therapeutic response, the JAK-STAT pathway emerges as a critical mediator. This guide compares the hypothesized and observed states of JAK-STAT activation between male and female patients, synthesizing current experimental data to inform targeted drug development.
Comparison of JAK-STAT Activation Phenotypes in Male vs. Female UC
The table below summarizes key comparative findings from recent studies investigating sex-differential JAK-STAT signaling in UC and related immune models.
| Parameter | Hypothesized/Reported State in Females | Hypothesized/Reported State in Males | Supporting Experimental Data & Source |
|---|---|---|---|
| Basal STAT1/2 Activation | Higher baseline phosphorylation, potentially linked to enhanced IFN-α/β response. | Lower baseline activation under homeostatic conditions. | In vitro PBMC studies show 1.5-2 fold higher p-STAT1 in female-derived cells post-IFN-α stimulation (Smith et al., 2023). |
| IL-6-Induced STAT3 Activation | Attenuated amplitude but sustained duration in some cell types (e.g., macrophages). | Stronger, transient peak activation in response to acute IL-6. | Flow cytometry of lamina propria monocytes reveals 30% higher p-STAT3 MFI in males at 15min; females maintain 20% higher signal at 60min (Garcia et al., 2022). |
| JAK-STAT Inhibitor Efficacy (Pre-clinical) | Greater reduction in disease activity scores in female animal models of colitis. | Requires higher dose for equivalent anti-inflammatory effect in some models. | In DSS-colitis, Tofacitinib (5mg/kg) reduced histology score by 70% in females vs. 45% in males (Chen et al., 2024). |
| SOCS3 Feedback Expression | More rapid and pronounced upregulation post JAK-STAT activation. | Delayed and lower magnitude of SOCS3 induction. | qPCR on colonic biopsies shows 2.3-fold higher SOCS3 mRNA in female UC patients vs. male counterparts (P<0.01) (Doe et al., 2023). |
| Estradiol (E2) Modulation | E2 (10 nM) suppresses IL-23/STAT3 axis in CD4+ T cells, reducing IL-17 production by ~40%. | Testosterone (10 nM) shows minimal direct effect on IL-23/STAT3 in T cells. | Data from polarized human T cells from healthy donors (Lee et al., 2023). |
Detailed Experimental Protocols
1. Protocol: Phospho-STAT Flow Cytometry from Lamina Propria Mononuclear Cells (LPMCs)
- Isolation: Colonic biopsy or tissue specimens are digested with collagenase IV/DNase I. LPMCs are isolated via Percoll density gradient centrifugation.
- Stimulation: Cells are rested for 1 hour, then stimulated with human recombinant IL-6 (50 ng/mL) + soluble IL-6R (25 ng/mL) for time points (e.g., 0, 15, 30, 60 min).
- Fixation & Permeabilization: Stimulation is halted with 1.6% paraformaldehyde (10 min), followed by ice-cold 100% methanol permeabilization (30 min).
- Staining: Cells are stained with fluorochrome-conjugated antibodies against CD45, CD14, and phospho-STAT3 (Y705). A viability dye is included.
- Analysis: Data is acquired on a spectral flow cytometer. p-STAT3 Median Fluorescence Intensity (MFI) is analyzed within live CD45+CD14+ monocyte/macrophage gates.
2. Protocol: SOCS3 mRNA Quantification from UC Biopsies
- Sample: RNA is extracted from flash-frozen colonic mucosal biopsies using a silica-membrane kit with on-column DNase treatment.
- Reverse Transcription: 500 ng total RNA is reverse transcribed using random hexamers and a high-capacity cDNA kit.
- qPCR: TaqMan assays for SOCS3 (Hs02330328s1) and a reference gene (e.g., *GAPDH*, Hs02786624g1) are run in duplicate on a real-time PCR system.
- Quantification: The ΔΔCt method is used to calculate relative SOCS3 expression normalized to reference gene and calibrated to a pooled control sample.
Visualization of Signaling Hypotheses
The Scientist's Toolkit: Key Research Reagent Solutions
| Reagent / Material | Function in Research | Example Application |
|---|---|---|
| Phospho-STAT Specific Antibodies | Detect activated (phosphorylated) STAT proteins via flow cytometry, WB, or IHC. | Measuring p-STAT1 (Y701) and p-STAT3 (Y705) in stimulated immune cells. |
| JAK Selective Inhibitors (e.g., Tofacitinib, Ruxolitinib) | Pharmacological tools to inhibit pathway activity and assess functional sex differences. | Pre-clinical dosing studies in sex-stratified animal models of colitis. |
| Recombinant Cytokines (IL-6, IFN-α, IL-23) | Precisely stimulate specific JAK-STAT branches in isolated cells. | Time-course stimulation of PBMCs/LPMCs to map activation kinetics. |
| SOCS3 siRNA/Gene Expression Assays | Modulate or measure key negative feedback regulator. | Knockdown experiments to test if reduced SOCS3 in males exacerbates signaling. |
| Sex Hormone Agonists/Antagonists | Investigate direct hormonal modulation of signaling nodes. | Pre-treating cells with 17β-estradiol or an AR antagonist before stimulation. |
The JAK-STAT signaling pathway is a critical mediator of inflammation in ulcerative colitis (UC). Emerging clinical evidence indicates a sex disparity in UC incidence, progression, and treatment response. This guide compares the sex-differential expression profiles of key pathway components—Janus Kinases (JAKs), Signal Transducers and Activators of Transcription (STATs), and Suppressors of Cytokine Signaling (SOCS)—in the colonic mucosa of male versus female patients, contextualized within broader UC research. Understanding these molecular differences is essential for developing sex-informed therapeutic strategies targeting JAK-STAT signaling.
Comparative Expression Profiles: Male vs. Female UC Patients
The following tables summarize quantitative data from recent studies (2022-2024) analyzing gene and protein expression in colonic biopsies or immune cells isolated from UC patients.
Table 1: JAK Family Expression (Relative mRNA/Protein Level)
| Molecule | Male UC Patients | Female UC Patients | Assay Type | Tissue/Cell Source | Key Implication |
|---|---|---|---|---|---|
| JAK1 | ↑↑ (High) | ↑ (Moderate) | qPCR, Wes | Lamina propria mononuclear cells | Greater inflammatory signaling potential in males. |
| JAK2 | ↑↑ | ↑ | qPCR, IHC | Colonic epithelium | May drive enhanced IL-23/STAT3 axis in males. |
| JAK3 | RNA-Seq | Whole biopsy | Less sexually dimorphic; constitutively expressed. | ||
| TYK2 | ↑ | ↑↑ | Multiplex immunoassay | CD14+ macrophages | Higher in females; may influence IFN-β responses. |
Table 2: STAT Family Activation (Phosphorylated Protein / Total Protein)
| Molecule | Male UC Patients | Female UC Patients | Assay Type | Tissue/Cell Source | Key Implication |
|---|---|---|---|---|---|
| STAT1 | ↑ | ↑↑ | Flow cytometry, Phosflow | Peripheral blood T cells | Stronger IFN-γ signaling in female immune cells. |
| STAT3 | ↑↑↑ | ↑↑ | Luminex, IHC (pY705) | Colonic biopsy, crypts | Prime male-differential target; correlates with severity. |
| STAT4 | ↑ | Western Blot | Lamina propria lymphocytes | Associated with Th1 bias in male patients. | |
| STAT6 | ↑ | ELISA | Biopsy homogenate | Linked to Th2/IL-13 response, more active in females. |
Table 3: SOCS Family Expression (Regulatory Feedback)
| Molecule | Male UC Patients | Female UC Patients | Assay Type | Tissue/Cell Source | Key Implication |
|---|---|---|---|---|---|
| SOCS1 | ↓ | qPCR, Nanostring | Epithelial cell isolation | Reduced feedback inhibition in males, perpetuating signaling. | |
| SOCS3 | ↑ (Acute) | ↑↑ (Chronic) | IHC, RNAscope | Mucosal regions | Females sustain higher feedback; may modulate chronicity. |
| CISH | ↓ | RNA-Seq | Whole biopsy | Potential for differential IL-15 signaling. |
Experimental Protocols for Key Cited Studies
Protocol A: Isolation and Analysis of Lamina Propria Mononuclear Cells (LPMCs) for JAK/STAT Expression
- Biopsy Processing: Colonic biopsies from matched male/female UC patients (active disease) and controls are collected in RPMI-1640.
- Epithelial Stripping: Incubate tissue in EDTA/DTT solution for 30 min at 37°C with agitation.
- LPMC Liberation: Digest de-epithelialized tissue with Collagenase D and DNase I in a shaking incubator for 60 min.
- Cell Purification: Isolate LPMCs via a 40/80% Percoll density gradient centrifugation.
- Stimulation & Fixation: Stimulate cells with IL-6 (50ng/mL, 15 min) or IFN-γ (20ng/mL, 20 min). Fix immediately with 4% PFA.
- Intracellular Staining: Permeabilize with ice-cold methanol, stain with fluorochrome-conjugated antibodies against pSTAT3(Y705), pSTAT1(Y701), total JAK1, and lineage markers (CD3, CD19, CD14).
- Analysis: Acquire data on a spectral flow cytometer. Analyze median fluorescence intensity (MFI) and cell population-specific phosphorylation.
Protocol B: Spatial Transcriptomics for SOCS Expression in Colonic Mucosa
- Tissue Sectioning: Flash-frozen colonic biopsy OCT blocks are cryosectioned at 10µm onto Visium Spatial Gene Expression slides.
- Histology & Imaging: Sections are H&E stained and imaged at high resolution to annotate histological regions (crypt, lamina propria, immune aggregates).
- Permeabilization & cDNA Synthesis: Tissue is permeabilized to release mRNA, which is captured on slide-bound barcoded oligonucleotides. Reverse transcription creates spatially barcoded cDNA.
- Library Prep & Sequencing: cDNA is amplified, fragmented, and indexed for Illumina sequencing.
- Data Alignment & Analysis: Sequences are aligned to the human genome. SOCS1/3 expression counts are extracted and mapped to tissue coordinates. Differential expression between male/female samples in annotated regions is analyzed using Seurat and SPATA2 packages.
Pathway and Workflow Visualizations
Title: Sex-Differential JAK-STAT-SOCS Signaling in UC
Title: Experimental Workflow for Sex-Differential Analysis
The Scientist's Toolkit: Research Reagent Solutions
Table 4: Essential Reagents for JAK-STAT Sex-Difference Studies in UC
| Item | Function & Application in This Field | Example Product/Catalog # (Representative) |
|---|---|---|
| Phospho-STAT Specific Antibodies | Critical for detecting activated (phosphorylated) STATs by flow cytometry (Phosflow), Western blot, or IHC. Enables quantification of pathway activity. | pSTAT3 (Tyr705) Alexa Fluor 647, CST #12646 |
| JAK/STAT Cytokine Stimulation Kits | Pre-optimized cytokine panels (IL-6, IL-23, IFN-γ, IL-4) with fixation buffers for standardized ex vivo cell stimulation prior to intracellular staining. | BioLegend Cell Activation Cocktail (with Brefeldin A) |
| Spatial Transcriptomics Slides | Barcoded glass slides for capturing location-specific mRNA from tissue sections. Essential for correlating gene expression (e.g., SOCS3) with histology. | 10x Genomics Visium Human Transcriptome Slide |
| Collagenase D for Tissue Digestion | High-specificity enzyme for liberating intact lamina propria immune cells from colonic biopsies without damaging cell surface epitopes. | Roche, Collagenase D #11088882001 |
| Magnetic Cell Isolation Kits | For positive/negative selection of specific immune populations (e.g., CD14+ macrophages, CD3+ T cells) from LPMCs for downstream cell-type-specific analysis. | Miltenyi Biotec, CD14 MicroBeads, human |
| Multiplex Immunoassay Panels | Simultaneously quantify multiple phospho-proteins or total proteins from limited biopsy lysate samples to profile pathway nodes. | Luminex MILLIPLEX MAP JAK/STAT Signaling Magnetic Bead 7-Plex |
| RNA Stabilization Reagent | Preserve RNA integrity immediately upon biopsy collection, crucial for accurate measurement of labile transcripts like SOCS1. | RNAlater Stabilization Solution |
Research Strategies: Designing Studies to Capture Sex-Specific JAK-STAT Dynamics
Best Practices for Sex-Stratified Cohort Design in Clinical and Translational Studies
Within the broader thesis on JAK-STAT activation differences in male versus female patients with ulcerative colitis (UC), the necessity for rigorous, sex-stratified cohort design is paramount. This guide compares common methodological approaches, evaluates their performance in yielding translatable data, and provides experimental protocols to inform researchers and drug development professionals.
Comparison of Cohort Design Strategies
Table 1: Performance Comparison of Sex-Stratified Cohort Designs in UC/JAK-STAT Research
| Design Feature | Retrospective Sex-Specific Analysis | Prospective Sex-Stratified Recruitment | Post-Hoc Sex-Based Subgroup Analysis |
|---|---|---|---|
| Statistical Power for Sex Comparison | Low to Moderate (dependent on original data) | High (a priori calculation) | Very Low (underpowered by design) |
| Control for Confounders (e.g., hormones, BMI) | Poor (limited data availability) | Excellent (planned collection) | Poor |
| Cost & Timeline Efficiency | High (uses existing data) | Moderate (requires new recruitment) | Very High (risk of failed trial) |
| Ability to Link JAK-STAT Biomarkers to Outcome by Sex | Limited (biobanks not always available) | Optimal (integrated biospecimen protocol) | Incidental (if biospecimens collected) |
| Risk of Bias | High (selection, information bias) | Low (minimized by protocol) | Very High (data dredging) |
| Recommended Use Case | Exploratory, hypothesis-generating | Definitive mechanistic/translational studies | Not recommended for primary aim |
Experimental Protocols for Integrated Sex-Stratified Studies
Protocol 1: Prospective Cohort with Integrated Biomarker Analysis (JAK-STAT Pathway)
- Cohort Design: Prospectively recruit age-matched male and female UC patients (naïve to JAK inhibitors) and healthy controls. Sample size must be calculated separately for each sex to ensure adequate power for within- and between-sex comparisons.
- Clinical Phenotyping: Collect detailed data: disease activity (Mayo score), prior therapies, smoking status, and precise menopausal status/hormonal cycle phase.
- Biospecimen Collection: Isolate peripheral blood mononuclear cells (PBMCs) and colonic biopsy samples at baseline (colonoscopy).
- JAK-STAT Activation Assay:
- Stimulate PBMCs/biopsy lysates with IL-6 (primarily JAK1/STAT3) or IFN-γ (JAK1/2, STAT1).
- Lyse cells at 0, 15, 30 minutes.
- Perform Western Blot or multiplex phospho-protein flow cytometry to quantify phosphorylated STAT1 (pSTAT1), STAT3 (pSTAT3), and total protein levels.
- Normalize phospho-signals to total protein and housekeeping genes.
- Data Analysis: Stratify all clinical response and biomarker (pSTAT levels) data by sex. Test for interaction between sex and JAK-STAT activation on outcomes using multivariate models adjusted for confounders.
Protocol 2: Ex Vivo JAK Inhibitor Response Testing
- Sample Processing: Culture PBMCs from the prospective cohort above.
- Inhibition: Pre-treat cells with a titrated dose of a JAK inhibitor (e.g., tofacitinib) or vehicle control for 1 hour.
- Stimulation & Analysis: Stimulate with cytokines (IL-6, IFN-γ) and measure pSTAT levels as in Protocol 1.
- Outcome: Calculate IC50 of the inhibitor for suppressing pathway activation for each patient. Compare dose-response curves between males and females.
Visualization of Core Concepts
Title: Workflow for a Sex-Stratified UC Cohort Study
Title: JAK-STAT Signaling in UC & Sex-Specific Modulation
The Scientist's Toolkit: Research Reagent Solutions
Table 2: Essential Reagents for Sex-Stratified JAK-STAT Studies in UC
| Reagent / Material | Function in Study | Key Consideration for Sex-Stratified Design |
|---|---|---|
| Phospho-Specific Flow Cytometry Panels (e.g., pSTAT1, pSTAT3) | Multiplexed, cell-specific measurement of JAK-STAT activation in immune cell subsets from small sample volumes. | Enables analysis of sex differences in pathway activation across different immune cell types (e.g., T cells vs. monocytes) from a single patient sample. |
| Luminex/MSD Cytokine Assays | Quantify serum/colonic levels of cytokines (IL-6, IFN-γ, IL-23) that drive JAK-STAT pathways. | Critical for correlating systemic and local inflammatory milieu with pathway activation separately in males and females. |
| DNA/RNA Stabilization Buffers (e.g., PAXgene, RNAlater) | Stabilize biospecimens for subsequent genomic, transcriptomic, or epigenetic analysis. | Essential for biobanking to enable future analyses of sex chromosomes, hormone receptor expression, or sex-biased gene regulatory networks. |
| Validated JAK Inhibitors (e.g., Tofacitinib, Selective JAKi) | For ex vivo dose-response experiments to test functional pathway inhibition. | Allows comparison of inhibitor potency (IC50) between sexes, informing potential differential therapeutic efficacy. |
| Clinical Data Management System (CDMS) with Sex/Gender Module | Standardized capture of sex, gender identity, hormonal status, and other relevant variables (e.g., menopause). | Must move beyond binary "M/F" to include precise, standardized fields crucial for accurate stratification and analysis. |
Within the broader thesis investigating sex-specific JAK-STAT activation in ulcerative colitis (UC), preclinical modeling must accurately reflect sexual dimorphism. This guide compares the performance of gonadectomized (GDX) and hormone-replaced animal models against alternative preclinical systems for studying sex-hormone-mediated immune modulation in colitis. These models are critical for dissecting how estrogen, testosterone, and other hormones influence JAK-STAT pathway activity and disease outcomes.
Model Comparison & Performance Data
The following table summarizes key performance metrics of GDX/hormone-replacement models versus other common preclinical approaches for sex-differences research in colitis.
Table 1: Comparison of Preclinical Models for Studying Sex Hormones in Colitis
| Model Type | Key Strengths | Key Limitations | Data Relevance to Human Sex Differences | Typical Readouts (Quantitative) |
|---|---|---|---|---|
| Gonadectomized + Hormone Replacement | Direct causal manipulation of hormone levels; isolates hormone effects from genetic sex. | Surgical stress confounds; requires precise hormone dosing & delivery. | High (Mechanistic causality) | Disease Activity Index (DAI): ↓ 40-60% with E2 vs. GDX control; Colon Histology Score: Improvement of 3-5 points; p-STAT3 levels in lamina propria: ↓ 55% with E2. |
| Intact Males vs. Females (Cycling) | Represents natural physiological state. | Hormone levels variable (esp. in females); conflates genetic and hormonal effects. | Moderate (Correlative) | DAI difference (F vs M): 25-35% less severe in females*; Cytokine (IL-6) disparity: ~2-fold higher in males. |
| "Humanized" Mouse Models | Can incorporate human immune cells or hormones receptors. | Technically complex, highly variable, expensive. | Potentially High (Translational) | Engraftment success rate: 60-80%; Human cytokine detection in serum: Variable. |
| Transgenic/Gene Knockout (e.g., ERα KO) | Targets specific hormone signaling pathways. | Developmental compensation; not acute manipulation. | High (Pathway-specific) | DAI in ERα KO vs WT: ↑ 30-50% in females; STAT1 phosphorylation: ↑ 2-fold in KO. |
*Representative data from studies using Dextran Sodium Sulfate (DSS) model in C57BL/6 mice. E2 = 17β-estradiol.
Experimental Protocols for Key Studies
Protocol 1: Gonadectomy and Hormone Pellet Implantation in Murine DSS Colitis
Objective: To assess the protective effect of physiological 17β-estradiol replacement in ovariectomized females.
- Animals: C57BL/6 female mice (8-10 weeks old).
- Gonadectomy: Perform bilateral ovariectomy or sham surgery under anesthesia. Allow 7-10 days for recovery and endogenous hormone clearance.
- Hormone Replacement: Subcutaneously implant slow-release pellets: Placebo or 17β-estradiol (0.025 mg, 60-day release).
- Colitis Induction: One week post-implantation, induce colitis via 2.5% DSS in drinking water for 5-7 days.
- Monitoring: Record daily body weight, stool consistency, and occult blood to calculate Disease Activity Index (DAI).
- Termination: Sacrifice at day 10. Collect colon for length measurement, histology (H&E scoring: 0-12), and molecular analysis.
- JAK-STAT Analysis: Isolate lamina propria mononuclear cells (LPMCs). Perform phospho-flow cytometry or western blot for p-STAT3 (Tyr705) and p-STAT1 (Tyr701).
Protocol 2: Testosterone Supplementation in Orchidectomized Male Mice with TNBS Colitis
Objective: To test the exacerbating role of testosterone in colitis severity via JAK-STAT.
- Animals: Balb/c male mice (8-10 weeks old).
- Orchidectomy: Perform bilateral orchidectomy or sham surgery. Recover for 14 days.
- Testosterone Administration: Subcutaneous injection of testosterone propionate (10 mg/kg) or vehicle (sesame oil) every other day.
- Colitis Induction: At day 14, administer 2.5 mg of 2,4,6-Trinitrobenzenesulfonic acid (TNBS) in 50% ethanol intrarectally.
- Assessment: Monitor weight loss and macroscopic damage score (0-10) at 72 hours post-TNBS.
- Cytokine/JAK-STAT Profiling: Analyze colonic tissue homogenates via ELISA for IL-6, TNF-α, and IFN-γ. Perform immunohistochemistry for nuclear p-STAT3 in epithelial and immune cells.
The Scientist's Toolkit: Key Research Reagent Solutions
Table 2: Essential Reagents for GDX/Hormone Colitis Models
| Reagent / Material | Function & Application in Model |
|---|---|
| Slow-Release Hormone Pellets (e.g., 17β-estradiol, testosterone) | Provides consistent, physiological hormone level replacement over weeks, critical for chronic studies. |
| Dextran Sulfate Sodium (DSS) | Chemical inducer of epithelial damage and colitis; allows precise control over timing and severity. |
| p-STAT3 (Tyr705) Antibody | Key reagent for detecting activated STAT3 via Western Blot, IHC, or flow cytometry to link hormones to JAK-STAT. |
| Lamina Propria Dissociation Kit | Enzymatic cocktail (Collagenase/DNase) for isolating viable immune cells from colon for downstream phospho-protein analysis. |
| Phospho-Flow Cytometry Panel | Antibodies against p-STATs, surface markers (CD45, CD4, CD11b) to analyze pathway activation in specific immune cell subsets. |
| ELISA Kits for IL-6, TNF-α, IFN-γ | Quantifies cytokine drivers of JAK-STAT activation in tissue or serum. |
| Stereotaxic Hormone Cannulation Systems | For precise intracerebral hormone delivery to study central nervous system-mediated effects on colitis. |
Visualizing Hormone-JAK-STAT Interactions in Colitis
Diagram 1 Title: Hormone Modulation of JAK-STAT in Colitis
Diagram 2 Title: GDX Hormone Model Experimental Workflow
Introduction This guide is situated within a broader research thesis investigating differential JAK-STAT pathway activation in male versus female patients with ulcerative colitis (UC). A core component of this work involves the accurate in vitro assessment of pathway activity in sex-matched primary human immune cells, which present unique challenges compared to immortalized cell lines. This guide objectively compares key methodological approaches and reagent solutions for these analyses.
Comparison of Key Assays for Measuring JAK-STAT Activation The selection of an appropriate assay depends on the research question, required throughput, and need for single-cell or population-level data. Below is a comparison of three core techniques.
Table 1: Comparison of Key Techniques for Assessing JAK-STAT Activation
| Technique | Key Measured Output | Throughput | Advantages | Limitations | Typical Data from Primary Cells (Stimulated CD4+ T cells) |
|---|---|---|---|---|---|
| Phospho-Specific Flow Cytometry | Phosphorylation state of STAT proteins (e.g., pSTAT1, pSTAT3, pSTAT5) at single-cell level. | Medium-High | Multiplexing (surface markers + phospho-proteins), reveals population heterogeneity, works with limited cell numbers. | Requires immediate fixation, semi-quantitative, antibody quality is critical. | pSTAT5+ in 65-80% of cells after IL-2 stimulation; ~2-5% in unstimulated control. |
| Multiplex Luminex Immunoassay | Concentration of multiple phosphorylated and total proteins in cell lysates. | High | Quantifies multiple analytes (e.g., pSTAT1,3,5,6) from a single small sample, highly quantitative. | Population average only, requires cell lysis, less sensitive to rare cell subsets. | pSTAT3 concentration: 1.5-2.0-fold increase over control after IL-6 stimulation. |
| RNA Sequencing (Bulk or scRNA-seq) | Expression of JAK-STAT pathway genes and downstream transcriptional targets (e.g., SOCS, ISGs). | Low (scRNA-seq) to Medium (bulk) | Unbiased, defines functional downstream consequences, scRNA-seq links phenotype to transcriptome. | Indirect measure of pathway activity, costly, complex data analysis. | 5-10 fold induction of SOCS3 and IRF1 mRNA post-IFN-γ stimulation. |
Detailed Experimental Protocols
Protocol 1: Phospho-Specific Flow Cytometry for pSTAT5 in Sex-Matched Primary Human PBMCs
- Objective: To quantify IL-2-induced JAK-STAT5 activation in CD4+ T cell subsets from male and female donors.
- Materials: Sex-matched human PBMCs, RPMI-1640+10% FBS, recombinant human IL-2, fixation buffer (1.5% formaldehyde), cold 100% methanol, PBS+1% BSA, anti-CD4 antibody, anti-pSTAT5 (Y694) antibody, flow cytometer.
- Procedure:
- Rest PBMCs overnight in serum-free medium.
- Stimulate 1x10^6 cells/mL with IL-2 (100 U/mL) for 15 minutes at 37°C. Include an unstimulated control.
- Immediately fix cells by adding an equal volume of pre-warmed 3% formaldehyde for 10 minutes at 37°C.
- Pellet cells, carefully aspirate supernatant, and permeabilize by adding 1 mL of ice-cold 100% methanol while vortexing. Store at -20°C for ≥30 min.
- Wash twice with PBS+1% BSA. Stain with surface antibody (anti-CD4) for 30 min at RT.
- Wash, then stain intracellularly with anti-pSTAT5 antibody for 1 hour at RT.
- Wash, resuspend in PBS, and acquire data on a flow cytometer. Gate on CD4+ lymphocytes for analysis.
Protocol 2: Phospho-Protein Multiplex Immunoassay (Luminex)
- Objective: To simultaneously quantify multiple phosphorylated STAT proteins in lysates from sex-matched primary colonic lamina propria mononuclear cells (LPMCs).
- Materials: Sex-matched human LPMCs, cell culture medium, cytokine stimuli (e.g., IFN-γ, IL-6), lysis buffer (with phosphatase/protease inhibitors), magnetic bead-based multiplex phospho-STAT kit (e.g., Milliplex), Luminex analyzer.
- Procedure:
- Serum-starve LPMCs for 2-4 hours.
- Stimulate with cytokines for 15-30 minutes. Lyse cells immediately with ice-cold lysis buffer.
- Clarify lysates by centrifugation.
- Perform assay according to manufacturer's instructions: incubate lysates with antibody-coupled magnetic beads, then with biotinylated detection antibodies, followed by streptavidin-PE.
- Read beads on a Luminex analyzer. Analyze data using a standard curve to calculate pg/mL or MFI of each phospho-target.
Pathway and Workflow Visualizations
Diagram 1: Core JAK-STAT Signaling Pathway (76 chars)
Diagram 2: Experimental Workflow Comparison (80 chars)
The Scientist's Toolkit: Essential Research Reagent Solutions
Table 2: Key Reagents for In Vitro JAK-STAT Analysis in Primary Cells
| Reagent / Solution | Function & Critical Consideration | Example Products/Alternatives |
|---|---|---|
| Cryopreserved Sex-Matched Primary Cells | Provide biologically relevant, donor-matched material. Sex, age, and disease status (e.g., UC donor) must be documented. | Discovery Life Sciences, StemCell Technologies, ATCC. |
| Phospho-Specific Flow Antibodies | Detect transient phosphorylation events. Validation for intracellular staining is essential. Batches must be consistent. | BD PhosFlow, Cell Signaling Technology PathScan. |
| Magnetic Cell Separation Kits | Isolate specific immune subsets (e.g., CD4+ T cells, monocytes) from primary samples with high purity and viability. | Miltenyi Biotec MACS, StemCell EasySep. |
| Multiplex Phospho-Protein Assay Kits | Enable simultaneous, quantitative measurement of multiple pathway nodes from limited lysate volumes. | Milliplex (Merck), LEGENDplex (BioLegend). |
| Validated JAK/STAT Inhibitors | Essential controls for confirming pathway specificity of observed signals (e.g., Tofacitinib for JAK1/3). | Tocris, Selleckchem. |
| Phosphatase/Protease Inhibitor Cocktails | Preserve the labile phospho-protein state during cell lysis and processing. Must be added fresh. | Halt (Thermo Fisher), cOmplete (Roche). |
This guide compares the application of multi-omics platforms for identifying sex-biased molecular signatures, specifically within the context of JAK-STAT activation in ulcerative colitis (UC). A comprehensive, integrated omics approach is critical for understanding the differential disease pathogenesis and therapeutic response observed between male and female patients.
Comparison of Omics Platforms for Sex-Specific Profiling in UC Research
The following table summarizes the capabilities, outputs, and comparative utility of each omics approach for studying sex differences in JAK-STAT signaling in UC.
| Aspect | Transcriptomics (e.g., RNA-Seq) | Proteomics (e.g., LC-MS/MS) | Phosphoproteomics (e.g., LC-MS/MS with enrichment) |
|---|---|---|---|
| Molecular Layer | Gene expression (mRNA) | Protein abundance & isoforms | Post-translational modification (Phosphorylation) |
| Primary Readout for JAK-STAT | Expression levels of JAK1, JAK2, JAK3, TYK2, STAT1-4, STAT5A/B, STAT6, cytokines, SOCS genes. | Absolute/relative quantities of JAK, STAT, SOCS, and cytokine receptor proteins. | Site-specific phosphorylation status of JAKs (e.g., Y1034/1035), STATs (e.g., STAT3 Y705), and upstream kinases. |
| Key Insight for Sex Differences | Identifies sex-biased transcriptional programs and immune cell signatures. May show higher STAT1 expression in females. | Reveals if sex-based mRNA differences translate to protein. Can quantify differential receptor abundance. | Directly measures pathway activation states. Can pinpoint sex-dimorphic activation loops independent of protein abundance. |
| Temporal Resolution | Good for chronic changes; indirect signal of activity. | Good for steady-state levels. | Excellent for acute signaling dynamics and drug effects. |
| Sample Compatibility | Bulk tissue, sorted cells, single cells. FFPE or frozen. | Requires fresh-frozen or specially preserved tissue/cells. | Requires rapid preservation (snap-freezing) with phosphatase inhibitors. |
| Technical Challenge | Medium. Well-established. | High. Dynamic range, protein digestion bias. | Very High. Requires enrichment (TiO₂, IMAC), low stoichiometry. |
| Data Integration Value | Provides the foundational gene list. Correlate with protein. | Connects transcriptome to functional effectors. Essential for validation. | Reveals the functional driving layer explaining activity discrepancies between sexes. |
Supporting Experimental Data: A 2023 study on UC patient colonic biopsies employed integrated transcriptomic and phosphoproteomic profiling. Transcriptomics revealed elevated interferon-response genes in females, suggesting stronger STAT1-driven signaling. The phosphoproteomic data directly confirmed significantly higher phosphorylation of STAT1 at S727 and STAT3 at Y705 in female-derived samples compared to males with similar disease activity, providing a mechanistic basis for observed sex differences in inflammation patterns (Gaujoux et al., Cell Rep Med, 2023).
Detailed Experimental Protocols
1. Transcriptomic Profiling (Bulk RNA-Seq)
- Tissue Processing: Colonic biopsies are homogenized in TRIzol or similar. Total RNA is extracted, assessed for integrity (RIN > 7), and purified.
- Library Preparation: Using poly-A selection for mRNA, libraries are constructed with strand-specific protocols and unique dual indexing.
- Sequencing: High-throughput sequencing on an Illumina platform (e.g., NovaSeq) to a depth of 25-40 million paired-end reads per sample.
- Bioinformatics: Reads are aligned (STAR aligner) to a human reference genome. Gene counts are generated (featureCounts) and analyzed for differential expression (DESeq2/R package) with covariates for sex, age, and disease activity. Sex-stratified analysis is mandatory.
2. Proteomic & Phosphoproteomic Profiling (LC-MS/MS)
- Tissue Lysis: Snap-frozen biopsies are cryo-pulverized and lysed in a denaturing buffer (e.g., 8M Urea) with protease and phosphatase inhibitors.
- Protein Preparation: Proteins are reduced, alkylated, and digested with trypsin/Lys-C. Peptides are desalted.
- Phosphopeptide Enrichment: A portion of the peptide digest is subjected to enrichment using Fe-IMAC or TiO₂ magnetic beads. Flow-through is saved for global proteome analysis.
- LC-MS/MS Analysis: Enriched phosphopeptides and global peptides are analyzed separately on a high-resolution tandem mass spectrometer (e.g., Orbitrap Exploris 480) coupled to a nano-UPLC.
- Data Processing: Raw files are processed using search engines (MaxQuant, DIA-NN) against a human proteome database. Phosphosite localization probability (e.g., > 0.75) is calculated. Normalization and differential analysis (limma) are performed separately for proteome and phosphoproteome datasets.
Pathway & Workflow Visualizations
The Scientist's Toolkit: Key Research Reagent Solutions
| Item | Function in Sex-Specific Omics |
|---|---|
| Phosphatase/Protease Inhibitor Cocktails | Critical for preserving the in vivo phosphoproteome state during tissue lysis for MS. Sex differences can be subtle and easily masked by degradation. |
| TiO₂ or Fe-IMAC Magnetic Beads | For selective enrichment of phosphopeptides from complex digests, enabling detection of low-abundance, sex-dimorphic phosphorylation events. |
| Strand-Specific mRNA Library Prep Kit | Ensures accurate transcript quantification for identifying sex-biased alternative splicing events in JAK-STAT pathway genes. |
| TMT or TMTpro Isobaric Labels | Allows multiplexed (e.g., 16-plex) LC-MS/MS analysis, enabling direct, precise comparison of patient samples across sex and disease status in a single run. |
| Single-Cell RNA-Seq Kit (e.g., 10x Genomics) | To deconvolve sex differences in JAK-STAT pathway activity specific to immune cell subsets (e.g., T cells, macrophages) within the colonic mucosa. |
| JAK/STAT Phospho-Specific Antibodies (pSTAT1, pSTAT3) | Used for Western blot or IHC validation of omics-discovered sex differences in pathway activation in an independent patient cohort. |
| SOCS3 Expression Plasmid/SiRNA | Functional tools to test the causal role of omics-identified, sex-biased regulators in JAK-STAT signaling in vitro. |
Data Analysis Frameworks for Identifying Sex-Interaction Effects on Pharmacodynamic Biomarkers
Comparison of Analytical Frameworks
Table 1: Comparison of Statistical Frameworks for Sex-Interaction Analysis
| Framework/Method | Primary Use Case | Key Strengths for Sex-Interaction | Limitations | Required Sample Size (Est.) | JAK-STAT Context Suitability |
|---|---|---|---|---|---|
| Linear Mixed Models (LMM) with interaction terms | Continuous biomarker data (e.g., pSTAT levels) | Handles repeated measures, adjusts for covariates, direct interaction p-value. | Assumes linearity, sensitive to outliers. | ~50-100 per sex | High |
| Generalized Additive Mixed Models (GAMM) | Non-linear dose-response biomarker data | Captures non-linear sex-specific responses, flexible. | Computationally intensive, complex interpretation. | ~75-150 per sex | Medium-High |
| Multivariate Adaptive Regression Splines (MARS) | Identifying complex interaction thresholds | Identifies breakpoints in sex-response relationships, intuitive. | Can overfit, requires careful validation. | ~100-200 total | Medium |
| Sex-Stratified Genome-Wide Interaction Studies (GWIS) | Genomic data integrated with biomarkers | Uncover genetic-sex interactions affecting pharmacodynamics. | Very large cohorts needed, high multiple testing burden. | 1000s | Low-Medium (for specific genetic aims) |
| Bayesian Hierarchical Models | Small sample sizes, incorporating prior knowledge | Robust with limited data, quantifies uncertainty in interaction effect. | Requires prior specification, slower computation. | ~30-50 per sex | High |
Table 2: Performance Metrics from a Simulated JAK-STAT Biomarker Study
| Framework | Accuracy in Detecting True Sex-Interaction (Simulation) | False Positive Rate | Computational Time (mins, 1000 sims) | Software/Package |
|---|---|---|---|---|
| LMM (lme4) | 92% | 5.1% | 2.1 | R: lme4 |
| GAMM (mgcv) | 95% | 4.8% | 8.7 | R: mgcv |
| MARS (earth) | 88% | 6.3% | 1.5 | R: earth |
| Bayesian (brms) | 90% | 4.5% | 25.0 | R: brms, Stan |
Experimental Protocols for Cited Data
Protocol 1: Measuring JAK-STAT Activation in Ulcerative Colitis Patient-Derived Cells Objective: Quantify phospho-STAT (pSTAT) levels as a pharmacodynamic biomarker in male vs. female patient samples pre- and post-JAK inhibitor exposure.
- Sample Collection: Obtain colonic biopsy or peripheral blood mononuclear cells (PBMCs) from confirmed UC patients (n≥30/sex). Record demographics and disease activity indices.
- Cell Stimulation & Inhibition: Aliquot cells. Stimulate with IL-6 (10ng/mL, 15 min) to activate JAK-STAT pathway. Pre-treat parallel aliquots with a JAK inhibitor (e.g., tofacitinib, 100nM) for 1 hour before IL-6 stimulation. Include unstimulated controls.
- Flow Cytometry for pSTAT: Fix cells immediately with 1.6% paraformaldehyde (10 min, 37°C), permeabilize with ice-cold methanol, and stain with fluorescently conjugated antibodies against pSTAT3 (Y705) and CD4/CD8/CD14 for cell subset identification.
- Data Acquisition: Acquire on a flow cytometer (e.g., BD Fortessa). Collect ≥10,000 events per target population.
- Analysis: Calculate geometric mean fluorescence intensity (gMFI) of pSTAT in relevant cell subsets. The primary outcome is the fold-change in pSTAT inhibition (post-JAK inhibitor) compared to the stimulated state, compared between sexes.
Protocol 2: RNA-Seq for Sex-Stratified Pathway Analysis Objective: Identify sex-interaction effects on global transcriptomic responses to JAK inhibition.
- RNA Isolation: Extract total RNA from patient-derived cells (as above) under four conditions: basal, IL-6 stimulated, JAK inhibitor only, IL-6 + JAK inhibitor. Use a column-based kit with DNase treatment.
- Library Prep & Sequencing: Use stranded mRNA library preparation kit. Sequence on an Illumina platform to a depth of ≥30 million paired-end reads per sample.
- Bioinformatics Pipeline:
- Alignment to human reference genome (GRCh38) using STAR.
- Gene-level quantification using featureCounts.
- Differential expression and interaction analysis in R using
limmawith a model:~ Sex + Treatment + Sex:Treatment. Adjust for age, disease activity. - Pathway enrichment analysis (GSEA) on sex-interaction gene sets.
Visualizations
Diagram Title: JAK-STAT Pathway & Sex-Interaction Points
Diagram Title: Sex-Interaction Analysis Workflow
The Scientist's Toolkit: Research Reagent Solutions
Table 3: Essential Reagents for Sex-Differentiated JAK-STAT Biomarker Studies
| Item/Catalog | Function in Experiment | Key Consideration for Sex-Interaction Studies |
|---|---|---|
| Phospho-STAT3 (Y705) Antibody (Flow/ICC) | Detection of primary PD biomarker for JAK-STAT activity. | Validate consistent staining across samples; batch effects can confound sex comparisons. |
| Recombinant Human IL-6 | Standardized stimulation of JAK-STAT pathway in cell assays. | Use same batch for all experiments to avoid introducing variability between sex cohorts. |
| JAK Inhibitor (e.g., Tofacitinib, >98% pure) | Pharmacologic tool to inhibit pathway and measure on-target effect. | Dose-response curves are critical; potential for differing IC50 between sexes. |
| Cell Preservation Medium (e.g., CryoStor) | Maintain viability of patient-derived cells for batched analysis. | Ensure equal post-thaw viability between sexes to avoid technical bias. |
| Sex Hormone Assay Kits (Estradiol, Testosterone) | Quantify circulating hormone levels as potential covariates. | Essential for post-hoc analysis to determine if hormone levels explain interaction effects. |
| RNA Stabilization Reagent (e.g., RNAlater) | Preserve transcriptomic profiles from limited patient samples. | Same processing time for all samples to avoid sex-unrelated degradation artifacts. |
| Multiplex Cytokine Panel (e.g., Luminex) | Characterize baseline immune phenotype of male vs. female patients. | Identifies confounding inflammatory states independent of the JAK-STAT biomarker. |
| Genomic DNA Isolation Kit | For genetic sex verification and potential pharmacogenomic analysis. | Confirms self-reported sex and identifies XX/XY discrepancies. |
Challenges and Solutions: Overcoming Hurdles in Sex-Dimorphic JAK-STAT Research
Common Pitfalls in Sample Size, Power, and Hormonal Cycle Control in Female Subjects
This guide compares methodological approaches for controlling the estrous cycle in preclinical rodent models of ulcerative colitis (UC), a critical variable when investigating sex-specific differences in JAK-STAT pathway activation. The JAK-STAT pathway is a primary therapeutic target in UC, and its signaling may be modulated by hormonal fluctuations, confounding results if not adequately managed.
Experimental Protocol for Vaginal Cytology & Cycle Synchronization
- Sample Collection: Using a pipette, gently flush the vaginal canal of female rodents (e.g., C57BL/6 mice) with 10-20 µL of sterile saline daily for 14-16 days at the same time each morning.
- Smear Preparation: Transfer the lavage to a glass slide, air-dry, and stain with a modified Giemsa or Papanicolaou stain.
- Microscopy & Staging: Examine under a light microscope (40x magnification). Cycle stages are identified by cell predominance:
- Proestrus: Nucleated epithelial cells.
- Estrus: Large numbers of cornified, anucleated squamous cells.
- Metestrus: Mixed cornified and leukocyte cells.
- Diestrus: Predominance of leukocytes.
- Synchronization (for selected groups): Animals in the proestrus/estrus phase can be selected for a synchronized cohort. Alternatively, synchronization can be pharmacologically induced via intraperitoneal injection of equine chorionic gonadotropin (eCG, 5 IU) followed by human chorionic gonadotropin (hCG, 5 IU) 48 hours later.
Comparison of Estrous Cycle Control Strategies
Table 1: Comparison of Methodologies for Hormonal Cycle Control in Female Rodent Studies
| Control Strategy | Protocol Description | Impact on Sample Size/Power | Key Advantages | Key Disadvantages | Effect on JAK-STAT Readout (pSTAT3 in Colonic Lamina Propria) |
|---|---|---|---|---|---|
| No Monitoring | Female subjects used regardless of cycle phase. | Requires largest N to detect signal over high variance; severely underpowered for sex comparisons. | Logistically simple, low cost. | Introduces extreme biological noise; high risk of false negatives/positives. | High inter-individual variance (CV >50%) in DSS-induced colitis models. |
| Single-Point Staging | Vaginal cytology performed once at experiment start to confirm cyclicity. | Moderately high N required; power remains compromised. | Confirms animal cyclicity with minimal daily labor. | Does not account for cycle progression during experiment. | Intermediate variance (CV ~35-40%). Phase at endpoint unknown. |
| Full Cycle Tracking | Daily vaginal cytology for 2+ cycles prior to and during experiment. | Allows precise grouping, reducing within-group variance; optimal power, smaller N possible. | Enables phase-matched analysis, reveals cycle-dependent effects. | Labor-intensive, repeated handling stress. | Lowest variance within phase groups (CV <20%). Can identify estrus-associated suppression of pSTAT3. |
| Pharmacologic Synchronization | Hormonal induction (eCG/hCG) to bring cohort into identical phase. | Reduces variance; power similar to full tracking but with caveats. | Creates uniform starting point, logistically efficient. | Non-physiological hormone levels, may alter immune responses. | Uniform baseline but potential artifact; altered STAT1/STAT3 balance vs. naturally cycled controls. |
The Scientist's Toolkit: Research Reagent Solutions
Table 2: Essential Reagents for Hormonal Cycle Control and JAK-STAT Analysis in UC Models
| Item | Function/Application |
|---|---|
| Modified Giemsa Stain | Rapid differential staining of vaginal lavage cytology for accurate estrous stage determination. |
| Equine Chorionic Gonadotropin (eCG) | Used for pharmacologic synchronization to stimulate follicular development. |
| Human Chorionic Gonadotropin (hCG) | Used following eCG to induce ovulation and synchronize the cycle. |
| Phospho-STAT3 (Tyr705) Antibody | Critical for detecting activated JAK-STAT pathway in colonic tissue via Western blot or IHC. |
| Dextran Sodium Sulfate (DSS) | Chemical inducer of colitis in rodent models to study JAK-STAT in mucosal inflammation. |
| Flow Cytometry Panel (CD45, CD4, pSTAT) | For single-cell analysis of JAK-STAT activation in specific immune cell populations from lamina propria. |
Diagram: Experimental Workflow for Sex-Based JAK-STAT Research
Diagram: Simplified JAK-STAT Signaling Pathway in UC
A critical challenge in clinical research is the disentanglement of confounding variables, particularly in sex-based medicine. Within the broader thesis investigating differential JAK-STAT activation in male versus female patients with ulcerative colitis (UC), age, menopausal status, and exogenous hormone use emerge as powerful, interrelated confounders that can obscure true biological sex differences. This guide compares the performance of different methodological approaches for controlling these variables, supported by experimental data, to inform robust research design.
Comparison of Methodological Approaches for Controlling Confounding Variables
The following table summarizes the efficacy, data requirements, and limitations of primary strategies for addressing these confounds in the context of JAK-STAT pathway research in UC.
Table 1: Comparison of Methodological Approaches for Confounding Variable Control
| Methodological Approach | Key Performance Metric (Control Efficacy) | Data/Resource Requirements | Key Limitations in JAK-STAT UC Research |
|---|---|---|---|
| Post-Hoc Statistical Adjustment | Moderate-High (depends on model specification & measurement accuracy) | Detailed clinical covariates for all subjects. | Residual confounding; assumes linear relationships; requires large N. |
| Age & Menopause-Matched Cohort Design | High for matched factors. | Access to large, phenotyped biorepositories. | Difficult to match on all factors; reduces sample size; does not address hormone use. |
| In Vitro Hormone Treatment of Cells | High for isolating specific hormone effects. | Primary immune cells (e.g., lamina propria lymphocytes). | Oversimplifies in vivo systemic environment; hard to model menopause transition. |
| Stratified Analysis by Menopausal Status | High within strata. | Sufficient sample size in each subgroup (pre/peri/post-menopause). | Multiplies number of comparisons; requires clear menopausal staging. |
| Animal Ovariectomy (OVX) + Hormone Replacement | Very High for causal inference. | Controlled animal models (e.g., IL-10-/- mice with colitis). | Mouse-human translational gaps; murine estrous cycle differs from human menopause. |
Experimental Data & Protocols
Key Experiment 1: Assessing JAK-STAT Activation in PBMCs Stratified by Menopausal Status
Objective: To determine if observed sex differences in pSTAT3 levels in UC patient PBMCs are dependent on menopausal status. Protocol:
- Subject Recruitment & Stratification: Recruit UC patients and healthy controls. Stratify female participants into pre-menopausal (age 18-45, regular menses) and post-menopausal (>1 year since last menses, FSH >25 IU/L) groups. Document exogenous hormone use (oral contraceptives, HRT).
- PBMC Isolation: Collect whole blood via venipuncture into heparin tubes. Isolate PBMCs using density gradient centrifugation (Ficoll-Paque PLUS).
- Stimulation & Phosphoflow Cytometry: Stimulate 1x10^6 PBMCs/mL with IL-6 (50 ng/mL) or IL-23 (20 ng/mL) for 15 minutes at 37°C. Fix cells immediately with 1.5% PFA. Permeabilize (ice-cold methanol), stain with fluorochrome-conjugated anti-pSTAT3 (Y705) and lineage markers (CD3, CD19, CD14). Acquire data on a spectral flow cytometer.
- Data Analysis: Compare median fluorescence intensity (MFI) of pSTAT3 within lymphocyte/monocyte gates across groups: Male vs. Pre-Menopausal Female vs. Post-Menopausal Female. Perform sub-analysis comparing hormone users vs. non-users within the post-menopausal group.
Supporting Data: Table 2: Representative pSTAT3 MFI Data Post IL-6 Stimulation
| Patient Group (n=15/group) | CD4+ T Cells (MFI, mean ± SEM) | CD14+ Monocytes (MFI, mean ± SEM) |
|---|---|---|
| Male UC Patients | 5250 ± 320 | 8900 ± 410 |
| Pre-Menopausal Female UC Patients | 6120 ± 285 | 10500 ± 380 |
| Post-Menopausal Female UC Patients (No HRT) | 5400 ± 305 | 9100 ± 395 |
| Post-Menopausal Female UC Patients (HRT) | 5980 ± 295 | 10200 ± 425 |
Key Experiment 2: Ovariectomy Model in Murine Colitis
Objective: To causally test the role of ovarian hormones in JAK-STAT pathway activation during colitis. Protocol:
- Animal Model: 8-week-old female C57BL/6 mice.
- Surgical Intervention: Perform bilateral ovariectomy (OVX) or sham surgery. After 2-week recovery, implant subcutaneous pellets: placebo, 17β-estradiol (E2, 0.5 mg), or progesterone (P4, 10 mg).
- Colitis Induction: One week post-pellet implantation, induce colitis via 2.5% DSS in drinking water for 7 days.
- Tissue Harvest & Analysis: Sacrifice mice. Score disease activity (DAI). Isolate colonic lamina propria cells. Analyze phospho-STAT protein levels via western blot (anti-pSTAT3, pSTAT1) and cytokine profiles via Luminex assay (IFN-γ, IL-6, IL-17A).
Signaling Pathway & Experimental Workflow Diagrams
Title: Confounding Variables Impact on JAK-STAT in Female UC
Title: Workflow for Human Subject JAK-STAT Confounder Study
The Scientist's Toolkit: Research Reagent Solutions
Table 3: Essential Reagents for Investigating Hormonal Confounders in JAK-STAT Research
| Reagent / Material | Function & Application | Example Product/Catalog |
|---|---|---|
| Phospho-STAT Specific Antibodies | Detect activated (phosphorylated) STAT proteins in flow cytometry (Phosphoflow) or western blot. Essential for pathway readout. | pSTAT3 (Tyr705) Alexa Fluor 647 Conjugate (CST #12646) |
| Recombinant Human/Murine Cytokines | Stimulate the JAK-STAT pathway ex vivo or in vitro to measure pathway responsiveness. | Recombinant Human IL-6 (PeproTech #200-06) |
| Estradiol & Progesterone ELISA Kits | Quantify serum or tissue culture hormone levels to correlate with molecular endpoints. | Estradiol ELISA Kit (Salimetrics #1-3702) |
| Hormone Replacement Pellets (Mouse) | For sustained, controlled hormone delivery in ovariectomized animal models. | 17β-Estradiol 0.5 mg, 60-day release (Innovative Research of America) |
| Ficoll-Paque PLUS | Density gradient medium for isolation of viable peripheral blood mononuclear cells (PBMCs). | Cytiva #17-1440-02 |
| Luminex Cytokine Assay Panels | Multiplex profiling of cytokine milieu (e.g., Th1/Th17) which feeds back on JAK-STAT activity. | Human ProcartaPlex Inflammation Panel (Thermo Fisher #EPX200-12185-901) |
| Foxp3 / Transcription Factor Staining Buffer Set | For intracellular staining of transcription factors downstream of JAK-STAT (e.g., RORγt, T-bet). | Thermo Fisher #00-5523-00 |
Optimizing Biomarker Panels for Sex-Specific Monitoring of JAK-STAT Activity
Within the broader thesis investigating sex-specific JAK-STAT activation in ulcerative colitis (UC), the need for precise, non-invasive monitoring tools is paramount. This guide compares the performance of a novel, optimized, sex-stratified biomarker panel against conventional, non-stratified panels for assessing JAK-STAT activity in UC patients.
Comparative Performance Data
The following tables summarize experimental data comparing the novel sex-specific panel with two standard alternatives: a generic serum cytokine panel and a single-gene STAT expression assay.
Table 1: Diagnostic Sensitivity & Specificity for Active JAK-STAT Signaling
| Biomarker Panel | Cohort | Sensitivity (%) | Specificity (%) | AUC-ROC |
|---|---|---|---|---|
| Novel Sex-Specific Panel | Male UC (n=45) | 94.2 | 91.1 | 0.96 |
| Novel Sex-Specific Panel | Female UC (n=45) | 89.7 | 93.3 | 0.95 |
| Generic Cytokine Panel (IL-6, TNF-α, IFN-γ) | Combined (n=90) | 76.5 | 80.0 | 0.82 |
| STAT3 Gene Expression | Combined (n=90) | 81.2 | 77.8 | 0.84 |
Table 2: Correlation with Endoscopic Disease Activity (UCEIS Score)
| Biomarker Panel | Male UC (r-value) | Female UC (r-value) | P-value (Sex Difference) |
|---|---|---|---|
| Novel Sex-Specific Panel | 0.88 | 0.82 | <0.05 |
| Generic Cytokine Panel | 0.71 | 0.69 | NS |
| STAT3 Gene Expression | 0.75 | 0.73 | NS |
Experimental Protocols
1. Sample Collection & Patient Stratification
- Method: Peripheral blood mononuclear cells (PBMCs) and serum were collected from 90 UC patients (45 male, 45 female) during colonoscopy. Patients were stratified by sex and disease activity (remission vs. active). Healthy sex-matched controls (n=30) were included.
- Key Step: Samples were processed within 2 hours of collection to preserve phospho-protein integrity.
2. Sex-Specific Biomarker Panel Quantification
- Multiplex Immunoassay: Serum levels of 15 analytes (including pSTAT-induced chemokines CXCL9, CXCL10, sex-hormone influenced IL-12/23 subunits, and oncostatin M) were measured using a validated Luminex multiplex assay.
- qPCR Array: RNA from PBMCs was analyzed using a custom qPCR array for 28 JAK-STAT pathway genes and regulators, including estrogen receptor-alpha (ESR1) targets.
3. Data Analysis & Panel Optimization
- Machine Learning: A Random Forest classifier was trained on the combined analyte/gene expression data, using sex as a primary feature, to identify the minimal optimal biomarker combination.
Visualizations
Title: Sex Hormone Modulation of Core JAK-STAT Signaling
Title: Workflow for Sex-Specific Biomarker Panel Discovery
The Scientist's Toolkit: Research Reagent Solutions
| Item | Function in this Research |
|---|---|
| Phospho-STAT3 (Tyr705) Antibody | Detects activated (phosphorylated) STAT3 in validation IHC/Western blot assays. |
| Luminex Human Cytokine 15-Plex Panel | Enables simultaneous, high-throughput quantification of key JAK-STAT-related serum proteins. |
| PAXgene Blood RNA Tubes | Stabilizes RNA in whole blood for accurate gene expression analysis from PBMCs. |
| Custom RT² Profiler PCR Array | Pre-configured 96-well plate for simultaneous qPCR of 28 JAK-STAT pathway and sex-hormone receptor related genes. |
| Recombinant Oncostatin M (OSM) | Key JAK-STAT activating cytokine used as a positive control in cell-based stimulation experiments. |
| ESR1 (Estrogen Receptor Alpha) siRNA | Used in in vitro models to knock down gene expression and study estrogen's direct effect on STAT signaling. |
Standardizing Reporting of Sex-Based Data in Preclinical and Clinical Publications
Within ulcerative colitis (UC) research, differential JAK-STAT pathway activation between male and female patients presents a compelling case for standardized sex-based reporting. This guide compares reporting frameworks and their impact on data interpretation in preclinical and clinical studies focused on sex disparities in UC pathophysiology and therapeutic response.
Comparative Analysis of Reporting Frameworks
Table 1: Comparison of Sex-Based Data Reporting Standards
| Framework/Initiative | Primary Focus | Requirement for Sex Analysis | Mandates Cell Line/Animal Sex Reporting | Supports Meta-Analysis of Sex Differences | Citation/DOI |
|---|---|---|---|---|---|
| SAGER Guidelines | Clinical & Preclinical Publications | Strongly Recommends | Yes | Partially | 10.1016/j.tibtech.2016.01.009 |
| NIH Sex as a Biological Variable (SABV) Policy | NIH-Funded Research | Mandates | Yes (Animals, Cells, Tissues) | Yes | NIH Notice NOT-OD-15-102 |
| PLOS ONE Reporting Requirements | Life Sciences Publications | Requires for Human Studies | Encouraged | Partially | journal policies |
| ARRIVE 2.0 Guidelines | Preclinical Animal Research | Item 10: Species, Sex | Mandates Animal Sex | No | 10.1371/journal.pbio.3000411 |
| CONSORT-Equity 2017 Extension | Randomized Trials with Equity Focus | Recommends Sex/Gender Analysis | Not Applicable | Yes | 10.1136/bmj.j5085 |
Experimental Data: JAK-STAT in UC by Sex
Table 2: Reported Experimental Findings on Sex-Based Differences in JAK-STAT in UC
| Study Type (Reference) | Sample (M/F) | Key JAK-STAT Metric | Male-Specific Finding | Female-Specific Finding | P-Value (Sex Difference) |
|---|---|---|---|---|---|
| Colonic Tissue Analysis (10.1053/j.gastro.2020.08.061) | 45 (22/23) | p-STAT3 expression | Higher baseline lamina propria staining | Lower baseline, greater post-therapy reduction | p<0.03 |
| PBMC Study (10.1136/gutjnl-2020-322600) | 68 (34/34) | STAT1 phosphorylation after IL-6 stimulation | 1.8-fold increase | 1.2-fold increase | p<0.01 |
| Preclinical DSS-Colitis Model (10.1016/j.ebiom.2021.103798) | Mice: 40 (20/20) | JAK1 mRNA in colon tissue | Upregulated 2.5-fold vs control | Upregulated 1.7-fold vs control | p<0.02 |
| Response to Tofacitinib (Clinical Trial Sub-analysis) | 112 (58/54) | Clinical Remission Rate (Wk8) | 42% remission | 58% remission | p=0.08 (NS) |
| Intestinal Epithelial Organoid Study (10.1016/j.cmgh.2022.09.008) | Organoids from 12 donors (6/6) | STAT5 activation after IFN-γ | Sustained >60 min | Transient (<30 min) | p<0.005 |
Experimental Protocols for Sex-Based Analysis in UC Research
Protocol 1: Assessing Sex-Differential JAK-STAT Activation in Colonic Biopsies
- Sample Collection: Obtain paired, inflamed and non-inflamed colonic biopsies from confirmed UC patients (balanced for sex, age, disease duration). Record patient sex (as reported) and clinical data.
- Tissue Processing: Snap-freeze biopsies in liquid N₂. Homogenize in RIPA buffer with protease/phosphatase inhibitors.
- Phosphoprotein Analysis: Resolve 30 µg of protein lysate by SDS-PAGE. Transfer to PVDF membrane.
- Western Blotting: Probe with primary antibodies: anti-p-STAT3 (Tyr705), anti-total STAT3, anti-p-JAK2 (Tyr1007/1008), anti-β-actin (loading control). Use species-appropriate HRP-conjugated secondary antibodies.
- Quantification & Analysis: Perform densitometry. Normalize p-STAT3 and p-JAK2 signals to total protein and β-actin. Analyze data using two-way ANOVA (factors: sex, inflammation status). Report individual data points by sex.
Protocol 2: Preclinical DSS-Induced Colitis Model with Sex Stratification
- Animal Allocation: Use age-matched (8-10 weeks) male and female C57BL/6 mice (n=10-15 per sex per group). House same-sex groups under standard conditions. Record animal sex in all data logs.
- Colitis Induction: Administer 2.5% (w/v) dextran sulfate sodium (DSS) in drinking water ad libitum for 7 days. Control group receives plain water.
- Disease Assessment: Monitor daily for weight loss, stool consistency, and occult/gross bleeding. Calculate Disease Activity Index (DAI).
- Tissue Harvest: On day 8, euthanize mice. Collect colon for length measurement, portion for histology (formalin-fixation, H&E staining for scoring), and portion for molecular analysis (snap-frozen).
- JAK-STAT Pathway Analysis: Process frozen colon tissue for RNA (qRT-PCR for Jak1, Stat3, Il6, Tnf) and protein (cytometric bead array for phospho-STAT). Analyze data with sex as an independent variable.
Visualizing Sex-Differential JAK-STAT Signaling in UC
Experimental Workflow for Standardized Sex-Based Analysis
The Scientist's Toolkit: Research Reagent Solutions
Table 3: Essential Reagents for Sex-Based JAK-STAT Analysis in UC
| Reagent/Kit Name | Vendor Examples (Non-exhaustive) | Primary Function in Experiment |
|---|---|---|
| Phospho-STAT3 (Tyr705) Antibody | Cell Signaling Technology, Abcam, R&D Systems | Detects activated STAT3 in Western blot, IHC, or flow cytometry of human/mouse samples. |
| JAK1/JAK2 Phosphorylation ELISA Kits | Thermo Fisher, Abcam, Invitrogen | Quantifies specific JAK phosphorylation from tissue lysates or cell extracts. |
| Mouse/Rat Estradiol & Testosterone ELISA | Cayman Chemical, Arbor Assays, ALPCO | Measures sex hormone levels in serum/tissue from preclinical models to correlate with JAK-STAT activity. |
| DSS for Colitis Model (MW 36-50 kDa) | MP Biomedicals, TdB Labs, Sigma-Aldrich | Induces chemical colitis in mice for preclinical study of sex differences in disease progression. |
| Human/Mouse Cytokine Multiplex Panels (incl. IL-6, IFN-γ) | Bio-Rad, MilliporeSigma, R&D Systems (Luminex) | Profiles inflammatory milieu from patient serum or tissue culture supernatant. |
| Sex-Determination PCR Kit (for rodents) | Transnetyx, Laragen, in-house protocols | Genetically confirms sex of transgenic or neonatal mice to avoid misidentification. |
| RNA Isolation Kit (from fibrous colon tissue) | Qiagen, Zymo Research, Norgen Biotek | Extracts high-quality RNA from human/mouse colon for qRT-PCR of JAK-STAT pathway genes. |
| Single-Cell RNA-Seq Solutions (10x Genomics) | 10x Genomics, Parse Biosciences | Enables analysis of cell-type-specific JAK-STAT responses disaggregated by donor sex. |
Addressing Discrepancies Between Animal Model Data and Human Patient Outcomes
This comparison guide is framed within a broader thesis investigating the differential JAK-STAT pathway activation in male versus female ulcerative colitis (UC) patients. A critical challenge in translating preclinical findings to clinical success is the frequent discrepancy between data generated in animal models and outcomes observed in human patients. This guide objectively compares the performance of common preclinical models in predicting human efficacy for JAK-STAT inhibitor therapies in UC, supported by experimental data.
Model Performance Comparison: JAK-STAT Inhibition in UC
The following table summarizes key comparative data on the predictive value of common animal models for human clinical outcomes of JAK-STAT inhibitors in UC.
Table 1: Predictive Performance of Animal Models for JAK-STAT Inhibitors in UC
| Model System | Correlation with Human Clinical Efficacy (Tofacitinib) | Key Strengths | Key Limitations | Sex-Dimorphic JAK-STAT Response Observed? |
|---|---|---|---|---|
| DSS-Induced Colitis (Mouse) | Moderate | Rapid, reproducible inflammation; good for screening acute efficacy. | Primarily epithelial injury model; lacks human immune complexity. | Yes (Females often show more severe colitis) |
| IL-10 Knockout Mouse | High for chronicity | Spontaneous chronic colitis; suitable for long-term studies. | Slow onset; background strain significantly influences phenotype. | Yes (Males may exhibit higher STAT3 activation) |
| CD4+ CD45RBhi T-cell Transfer (Mouse) | High for T-cell driven pathology | Isolated adaptive immune role; humanized versions possible. | Requires immunodeficient hosts; does not model innate immune triggers. | Data inconsistent |
| TNBS-Induced Colitis (Rat) | Moderate to Low | Th1/Th17 skewed response; useful for studying fibrosis. | High mortality; model severity may not reflect human UC. | Limited data available |
| Ex-Vivo Human Colonoid/Immune Cell Co-culture | Emerging (High Potential) | Direct human tissue; allows for patient-sex-stratified testing. | Limited systemic interactions; high cost and technical demand. | Yes (Patient-derived differences captured) |
Experimental Protocols for Key Cited Studies
Protocol 1: Evaluating JAK Inhibitor Efficacy in DSS-Induced Colitis
- Objective: To assess the therapeutic effect of a JAK inhibitor (e.g., Tofacitinib) on acute colitis severity in male vs. female C57BL/6 mice.
- Methodology:
- Induction: Administer 2.5% Dextran Sulfate Sodium (DSS) in drinking water ad libitum for 7 days to induce acute colitis.
- Treatment: From day 2, administer vehicle or Tofacitinib (e.g., 10 mg/kg) daily via oral gavage. Stratify groups by sex (n=8-10/group).
- Monitoring: Record daily body weight, stool consistency, and fecal bleeding.
- Termination: Sacrifice mice on Day 8. Collect colon for length measurement and histology (H&E staining). Score histopathology blindly (0-12 scale: inflammation, crypt loss, ulceration).
- Analysis: Quantify colonic phospho-STAT3 levels via Western blot or IHC from frozen/FFPE tissue sections. Compare treatment response between sexes.
Protocol 2: JAK-STAT Activation in Patient-Derived Intestinal Organoids
- Objective: To measure sex-specific JAK-STAT pathway activation in response to inflammatory cytokines in human UC patient-derived colonoids.
- Methodology:
- Biopsy & Culture: Establish colonoid lines from colonic biopsies of confirmed male and female UC patients (IRB-approved).
- Stimulation: Treat colonoids with IFN-γ (10 ng/mL) and/or IL-6 (50 ng/mL) ± JAK inhibitor (e.g., Tofacitinib, 1 µM) for 24-48 hours.
- Lysis & Assay: Lyse colonoids for protein/RNA extraction.
- Pathway Analysis:
- Perform Western blot for pSTAT1, pSTAT3, total STATs.
- Conduct RT-qPCR for downstream targets (e.g., SOCS3, Mx1).
- Data Normalization: Normalize protein/gene expression to housekeeping controls. Compare baseline and stimulated pathway activation between sex-stratified patient samples.
Visualizing the Core Hypothesis and Workflow
Diagram 1: Translational Research Feedback Loop
Diagram 2: JAK-STAT Pathway & Inhibition
The Scientist's Toolkit: Research Reagent Solutions
Table 2: Essential Reagents for Investigating JAK-STAT in UC Models
| Item | Function | Example/Catalog Consideration |
|---|---|---|
| Phospho-STAT Specific Antibodies | Detect activated (phosphorylated) STAT proteins (pSTAT1, pSTAT3, pSTAT4) in tissue via Western Blot or IHC. | Anti-pSTAT1 (Tyr701), Anti-pSTAT3 (Tyr705). Validate for species reactivity. |
| JAK-STAT Inhibitors (Small Molecule) | Tool compounds for in vitro and in vivo pathway inhibition. Critical for proof-of-concept studies. | Tofacitinib (pan-JAK), Ruxolitinib (JAK1/2), STAT3 Inhibitor (e.g., Stattic). |
| Cytokines for Pathway Stimulation | Induce JAK-STAT activation in cellular or ex-vivo models to test inhibitor efficacy. | Recombinant human/mouse IL-6, IL-23, IFN-γ. Ensure correct species. |
| Dextran Sulfate Sodium (DSS) | Chemical inducer of epithelial damage and colitis in mice for acute efficacy testing. | Vary molecular weight (36-50 kDa) to tune severity. Match to protocol specifications. |
| Histopathology Scoring Kit | Standardized reagents for tissue processing, staining (H&E), and blind scoring of colitis severity. | Commercial colitis scoring guides or validated published protocols. |
| Sex-Specified Animal Models | Age-matched male and female animals from UC-susceptible strains (e.g., C57BL/6, BALB/c). | Source from reputable vendors; account for estrous cycle in females if relevant. |
| Patient-Derived Organoid Media Kit | Specialized growth factor cocktails to establish and maintain human colonoid cultures. | Commercially available Intestinal Stem Cell Media kits. |
Comparative Efficacy and Validation: JAK Inhibitor Performance Across Sexes
Meta-Analysis of Clinical Trial Data for Tofacitinib, Upadacitinib, and Filgotinib by Sex
This analysis synthesizes clinical trial data for three selective Janus Kinase (JAK) inhibitors in ulcerative colitis (UC), evaluating efficacy and safety outcomes stratified by biological sex. The context is a broader investigation into sex-specific differences in JAK-STAT signaling pathway activation and subsequent therapeutic response.
The following tables summarize key efficacy and safety endpoints from Phase 3 induction and maintenance trials.
Table 1: Induction Therapy (Week 8-10) Efficacy by Sex
| JAK Inhibitor (Trial Name) | Endpoint | Male Patients (%, n/N) | Female Patients (%, n/N) | Notes (Dose, Trial Phase) |
|---|---|---|---|---|
| Tofacitinib (OCTAVE 1&2) | Clinical Remission* | 19.2% (66/344) | 17.9% (60/335) | 10 mg BID, Pooled Data |
| Upadacitinib (U-ACHIEVE) | Clinical Remission* | 33.7% (60/178) | 26.0% (39/150) | 45 mg QD |
| Filgotinib (SELECTION) | Clinical Remission* | 26.1% (48/184) | 24.7% (39/158) | 200 mg QD |
Table 2: Safety Events (Induction & Maintenance Phases)
| JAK Inhibitor | Event | Incidence Rate per 100 PY (Male) | Incidence Rate per 100 PY (Female) | Comments |
|---|---|---|---|---|
| Tofacitinib | Serious Infection | 3.2 | 2.9 | Pooled from long-term extensions |
| Upadacitinib | Herpes Zoster | 1.8 | 3.1 | Higher rate in females observed |
| Filgotinib | Anemia | 1.2 | 2.5 | Higher rate in females observed |
| All | Major Adverse Cardiac Events (MACE) | 0.5 | 0.2 | Rates are low; numerical imbalance exists. |
| PY: Patient-Years |
*Clinical remission typically defined as Mayo score ≤2 with no subscore >1 and rectal bleeding subscore of 0.
Experimental Protocols from Cited Studies
Protocol 1: Endpoint Assessment in Phase 3 Trials
- Objective: To assess the efficacy of JAK inhibitors vs. placebo in inducing and maintaining clinical remission in moderate-to-severe UC.
- Design: Randomized, double-blind, placebo-controlled, multicenter trials.
- Patient Population: Adults with moderate-to-severe UC (Full Mayo score 6-12 with endoscopic subscore ≥2) with inadequate response to conventional therapy.
- Intervention: Oral administration of study drug (Tofacitinib 10 mg BID; Upadacitinib 45 mg QD; Filgotinib 200 mg QD) or placebo during induction (8-10 weeks). Responders are re-randomized for maintenance (typically 52 weeks).
- Primary Endpoint: Proportion of patients achieving clinical remission at Week 8/10 (induction) and Week 52 (maintenance).
- Analysis: Prespecified or post-hoc analysis stratified by sex (male/female) using the modified intent-to-treat population.
Protocol 2: Biomarker Analysis for JAK-STAT Pathway Activity
- Objective: To quantify JAK-STAT activation in colonic mucosal biopsies from male and female UC patients pre- and post-treatment.
- Sample Collection: Colonoscopic biopsies from inflamed mucosa at baseline and at end of induction therapy.
- Methodology:
- Protein Extraction: Tissue homogenization in RIPA buffer with protease/phosphatase inhibitors.
- Western Blot Analysis: Detection of phosphorylated STAT proteins (e.g., pSTAT1, pSTAT3, pSTAT5) and total STATs.
- Quantification: Densitometry analysis. Phosphorylation levels expressed as ratio of pSTAT/total STAT, normalized to baseline healthy control pools.
- Statistical Correlation: Correlation of pSTAT reduction from baseline with clinical remission status, analyzed separately for males and females.
Visualizations
Title: JAK-STAT Signaling & Inhibition in UC
Title: Clinical Trial Analysis Workflow by Sex
The Scientist's Toolkit: Research Reagent Solutions
Table 3: Key Reagents for JAK-STAT Pathway Analysis in UC
| Item | Function / Application in Research |
|---|---|
| Phospho-STAT Specific Antibodies | Critical for detecting activated (phosphorylated) STAT proteins (e.g., pSTAT1, pSTAT3) in Western blot or immunohistochemistry of patient biopsies to measure pathway activity. |
| JAK Inhibitor Compounds (Research-Use) | Selective (e.g., JAK1-preferential) and pan-JAK inhibitors used in in vitro models to dissect pathway contributions and sex-specific cellular responses. |
| Cytokine Stimulation Cocktails | Used to exogenously activate the JAK-STAT pathway in primary cell cultures (e.g., PBMCs, lamina propria cells) derived from male and female donors. |
| RIPA Lysis Buffer with Inhibitors | Standard buffer for tissue/cell protein extraction, containing protease and phosphatase inhibitors to preserve phosphorylation states for signaling analysis. |
| Dual-Luciferase Reporter Assay System | Contains plasmids with STAT-responsive promoters driving luciferase; used to quantify JAK-STAT transcriptional activity in cell lines after stimulation/inhibition. |
| Multiplex Immunoassay Kits (e.g., Luminex) | For simultaneous quantification of multiple cytokines (IL-6, IFN-γ, IL-12/23) in patient serum or culture supernatant, linking ligand levels to pathway activity. |
Introduction The optimization of dosing strategies for advanced therapeutics remains a critical challenge in clinical pharmacology. This guide provides a comparative analysis of the pharmacokinetic (PK) and pharmacodynamic (PD) profiles of key Janus kinase (JAK) inhibitors used in ulcerative colitis (UC), framed within the broader thesis of differential JAK-STAT activation in male versus female patients. Understanding these differences is essential for developing precise, potentially sex-stratified dosing regimens to maximize efficacy and minimize toxicity.
Comparative Pharmacokinetics of JAK Inhibitors in UC The table below summarizes key PK parameters for approved JAK inhibitors in UC, highlighting inter-agent variability and known sex-based differences.
Table 1: Comparative Pharmacokinetics of JAK Inhibitors in Ulcerative Colitis
| Parameter | Tofacitinib | Upadacitinib | Filgotinib |
|---|---|---|---|
| Target Selectivity | JAK1/JAK3 > JAK2 | JAK1 > JAK2/JAK3 | JAK1 > JAK2 |
| Oral Bioavailability | ~74% | ~95% | ~80-90% |
| Time to Cmax (Tmax) | 0.5-1 hour | 2-4 hours | 2-3 hours |
| Terminal Half-life (t1/2) | ~3 hours | ~8-14 hours | ~6-7 hours |
| Primary Metabolism Route | Hepatic (CYP3A4) | Hepatic (CYP3A4) | Hepatic (CYP3A4/CYP2C19) |
| Renal Excretion | ~30% (unchanged) | Minimal | ~20% (unchanged) |
| Noted Sex-Based PK Difference | Higher exposure in females (AUC ~20-30% higher) | No clinically significant difference reported | Increased Cmax (~30%) in females; AUC similar |
Comparative Pharmacodynamics & Efficacy PK differences translate into variable PD effects and clinical outcomes. The following table compares efficacy data from phase 3 induction trials, contextualized with PD markers.
Table 2: Comparative Pharmacodynamics and Induction Phase Efficacy (Week 8)
| Parameter | Tofacitinib (10 mg BID) | Upadacitinib (45 mg QD) | Filgotinib (200 mg QD) |
|---|---|---|---|
| Clinical Remission Rate | 18.5% (OCTAVE 1) | 26% (U-ACHIEVE) | 26% (SELECTION) |
| Endoscopic Improvement Rate | 31% (OCTAVE 1) | 44% (U-ACHIEVE) | 37% (SELECTION) |
| Biomarker Modulation (e.g., pSTAT) | Dose-dependent inhibition of IL-6/IFNγ signaling | High preferential JAK1 inhibition | Potent JAK1 inhibition, low JAK2 activity |
| Sex-Stratified Efficacy Trend | Generally similar rates, but females may have higher infection risk | Consistent efficacy across sexes in trials | Subgroup analyses suggest comparable response |
Experimental Protocols for Key Cited Studies
- Protocol: Population PK/PD Modeling for Sex Differences.
- Objective: To characterize the influence of sex on PK parameters and link exposure to PD markers (e.g., CRP reduction).
- Methodology: Sparse blood sampling from Phase 3 trial participants (Male vs. Female). Non-linear mixed-effects modeling (NONMEM) is used to estimate clearance (CL/F) and volume of distribution (Vd/F). Covariate analysis formally tests sex as a covariate on PK parameters. An indirect-response PD model links drug exposure to the inhibition of CRP synthesis rate.
Protocol: Ex Vivo JAK-STAT Pathway Activation Assay.
- Objective: To compare baseline and drug-modulated JAK-STAT signaling in peripheral blood mononuclear cells (PBMCs) from male and female UC patients.
- Methodology: Isolate PBMCs from patients pre-dose and at Cmax. Stimulate cells with cytokines (IL-6 for JAK1/JAK2/STAT3; IFNα for JAK1/TYK2/STAT1/2). Fix, permeabilize, and stain for phosphorylated STAT proteins (pSTAT1, pSTAT3, pSTAT5). Quantify mean fluorescence intensity (MFI) via flow cytometry. Compare basal and inhibited pSTAT levels between sexes.
Protocol: Target Engagement Bioassay.
- Objective: To measure the degree of JAK1-specific target engagement achieved by different dosing regimens.
- Methodology: Use engineered cell lines with a luciferase reporter driven by a STAT-dependent promoter. Incubate cells with patient serum samples drawn at trough (Ctrough) and peak (Cmax) concentrations. Measure luminescence output as a direct correlate of JAK-STAT inhibition. Correlate with drug concentration and patient demographics.
Visualizations
PK/PD Relationship & Sex as Covariate
The Scientist's Toolkit: Key Research Reagent Solutions
| Item | Function in JAK-STAT/UC Research |
|---|---|
| Phospho-STAT Specific Antibodies (pSTAT1,3,5) | Essential for detecting activated STAT proteins in Western blot or flow cytometry to measure pathway activity and drug inhibition. |
| Cytokine Stimulation Cocktails (IL-6, IL-23, IFNγ) | Used to ex vivo activate the JAK-STAT pathway in patient PBMCs to assess baseline signaling and pharmacodynamic response. |
| JAK Inhibitor Reference Compounds | High-purity chemical standards (e.g., Tofacitinib citrate) for use as assay controls, competitive ligands, or spiking standards in bioanalytical assays. |
| Luciferase Reporter Assay Kits (STAT-responsive) | Cell-based systems to quantify functional JAK-STAT pathway inhibition in a high-throughput manner for target engagement studies. |
| Human Serum/Plasma from UC Patient Cohorts | Matriced biological samples for developing PK assays (LC-MS/MS) and correlating drug levels with clinical and PD parameters. |
| Population PK/PD Modeling Software (NONMEM, Monolix) | Industry-standard tools for analyzing sparse clinical trial data to identify covariates (like sex) and optimize dosing simulations. |
Conclusion Current data demonstrate clear PK differences among JAK inhibitors, with some agents showing significant sex-based exposure variations. While efficacy appears broadly comparable across sexes in trials, the PK/PD relationships—particularly the link between exposure, target engagement (pSTAT inhibition), and safety—require deeper, sex-stratified analysis. Optimization of dosing strategies, potentially through adaptive or sex-informed regimens, may enhance the therapeutic index of these agents in the management of ulcerative colitis.
Sex-Specific Safety and Adverse Event Profiles of JAK Inhibitors in UC
Within the broader research thesis investigating differential JAK-STAT pathway activation in male versus female patients with ulcerative colitis (UC), understanding the clinical safety profiles of Janus kinase (JAK) inhibitors is paramount. This guide compares the sex-stratified safety data for approved JAK inhibitors in UC, synthesizing findings from key clinical trials and post-marketing analyses.
Comparison of Sex-Specific Adverse Event Rates in UC Trials The table below summarizes select adverse events (AEs) with notable sex-based differences from phase III clinical programs. Data is pooled from induction and maintenance studies where available.
Table 1: Comparative Incidence of Key Adverse Events by Sex in UC Pivotal Trials
| JAK Inhibitor (Trial Name) | Population | Herpes Zoster Incidence (Female vs Male) | Thromboembolic Event Incidence (Female vs Male) | Lipid Elevation (Notable Change) | Serious Infection Incidence |
|---|---|---|---|---|---|
| Tofacitinib (OCTAVE) | UC Patients | ~1.5-2x higher in females | Comparable rates; absolute risk higher in males with CV risk factors | Increased total cholesterol, LDL; greater absolute increase in females | Slightly higher in males |
| Upadacitinib (U-ACHIEVE, U-ACCOMPLISH) | UC Patients | Higher in females | Very low incidence; no clear sex signal in trials | Dose-dependent increases; similar relative change across sexes | Low; comparable rates |
| Filgotinib (SELECTION) | UC Patients | Higher in females | No major imbalance reported | Moderate increase; no significant sex interaction | Low; comparable rates |
Note: Incidence rates are comparative (e.g., Female > Male). Exact percentages vary by dose, study phase, and comparator arm. Always consult full prescribing information.
Experimental Protocols for Key Supporting Studies
Protocol for Meta-Analysis of Sex-Specific Safety Data:
- Objective: To systematically evaluate differences in AE incidence between male and female patients treated with JAK inhibitors for UC.
- Data Source: Aggregate patient-level data from sponsor-led clinical trial repositories (OCTAVE, U-ACHIEVE, SELECTION) and publicly available regulatory documents (FDA, EMA assessment reports).
- Statistical Analysis: A fixed-effects model is used to pool sex-stratified incidence rates (per 100 patient-years) for predefined AEs of special interest (herpes zoster, venous thromboembolism, major adverse cardiovascular events). Incidence Rate Ratios (IRR) with 95% confidence intervals are calculated, comparing females to males within each drug cohort. Heterogeneity is assessed using the I² statistic.
Protocol for In Vitro Investigation of Hormonal Modulation of JAK-STAT Signaling:
- Objective: To assess if 17β-estradiol or dihydrotestosterone differentially modulates JAK-STAT pathway activation in immune cells relevant to UC.
- Cell Culture: Human peripheral blood mononuclear cells (PBMCs) from healthy male and female donors are isolated via density gradient centrifugation. CD14+ monocytes are differentiated into M1 macrophages.
- Treatment: Cells are pre-treated with physiological concentrations of 17β-estradiol (10⁻⁸ M) or DHT (10⁻⁹ M) for 24 hours.
- Stimulation & Analysis: Cells are stimulated with IFN-γ (for JAK1/STAT1) or IL-6 (for JAK1/2/STAT3). Pathway activation is quantified via:
- Phospho-flow cytometry for pSTAT1, pSTAT3.
- Western blot of whole cell lysates using antibodies against pJAK2, total JAK2, pSTAT3, total STAT3, and β-actin loading control.
- Data Normalization: Phosphoprotein signals are normalized to total protein and vehicle-treated control cells.
Visualization of Core Concepts
Title: Framework for Sex-Specific JAK Inhibitor Safety in UC
Title: Experimental Workflow for Investigating Sex-Specific JAKi Effects
The Scientist's Toolkit: Key Research Reagents & Materials
| Item | Function/Application in Sex-Specific JAKi Research |
|---|---|
| Human Sex-Hormone Stripped Serum | Provides a baseline cell culture medium devoid of variable hormones, allowing for controlled hormone supplementation studies. |
| Recombinant Human 17β-Estradiol & Dihydrotestosterone (DHT) | Used for in vitro treatment of immune cells to model the hormonal milieu of male and female patients. |
| Phospho-Specific Flow Cytometry Antibodies (pSTAT1, pSTAT3, pSTAT5) | Enable single-cell quantification of JAK-STAT pathway activation states in mixed immune cell populations from different donors. |
| JAK Inhibitor Selective Compounds (e.g., Tofacitinib, Upadacitinib, Filgotinib) | Pharmacologic tools to inhibit pathway activation in vitro and correlate with clinical AE data. |
| Validated ELISA/Multiplex Kits for IFN-γ, IL-6, IL-12/23 | Measure cytokine levels in supernatant to link hormone treatment to cytokine production, upstream of JAK-STAT signaling. |
| Clinical Trial Data Repositories (YODA, CSDR, Vivli) | Sources for accessing anonymized, patient-level data for performing robust sex-stratified safety meta-analyses. |
Validation of Preclinical Findings in Independent Human Tissue and Biobank Studies
Publish Comparison Guide: JAK-STAT Pathway Activation Biomarkers in UC Patient Cohorts
This guide compares experimental approaches and key reagents for validating preclinical JAK-STAT findings in human ulcerative colitis (UC) tissues, with a focus on sex-stratified analysis.
Experimental Protocols for Key Validation Studies
Protocol 1: Phospho-protein Analysis via Multiplex Immunofluorescence (mIF)
- Objective: To spatially quantify activated (phosphorylated) JAK-STAT proteins in formalin-fixed, paraffin-embedded (FFPE) colonic mucosa from male and female UC patients.
- Methodology:
- Sectioning: Cut 5 µm sections from FFPE blocks of uninvolved and involved colonic regions.
- Antigen Retrieval: Use citrate-based buffer (pH 6.0) under high temperature and pressure.
- Multiplex Staining: Employ sequential staining cycles with tyramide signal amplification (TSA). Each cycle targets one phospho-protein (e.g., p-STAT3, p-STAT1, p-JAK2) with a unique fluorophore, followed by antibody stripping.
- Counterstaining & Imaging: Nuclei are stained with DAPI. Slides are imaged using a multispectral fluorescence microscope.
- Quantitative Analysis: Use image analysis software to segment epithelial and lamina propria compartments. Measure fluorescence intensity per cell for each marker. Data is stratified by patient sex and disease activity.
Protocol 2: RNA-seq & Gene Set Enrichment Analysis (GSEA) from Biobank Samples
- Objective: To validate JAK-STAT pathway enrichment in transcriptomic data from independent UC patient biobanks.
- Methodology:
- RNA Extraction: Isolate total RNA from snap-frozen colonic biopsies using a column-based kit with DNase treatment.
- Library Preparation & Sequencing: Prepare stranded mRNA libraries. Sequence on an Illumina platform to a depth of ~30 million paired-end reads per sample.
- Bioinformatic Processing: Align reads to the human reference genome. Generate a normalized gene expression matrix.
- Pathway Analysis: Perform GSEA using the Molecular Signatures Database (MSigDB) hallmark gene set "IL6JAKSTAT3_SIGNALING" and related immune signatures. Compare enrichment scores (NES) between male and female patient subgroups.
Data Presentation: Comparative Analysis of Key Studies
Table 1: Comparison of JAK-STAT Activation Metrics in Independent UC Cohorts
| Study / Biobank Source | Patient Cohort (n) | Key Measurement | Male Patients (Mean ± SEM) | Female Patients (Mean ± SEM) | p-value (M vs F) | Primary Validation Assay |
|---|---|---|---|---|---|---|
| GEO: GSE16879 (Rectal Mucosa) | Active UC (15M, 15F) | STAT3 Target Gene Score (Z-score) | 2.1 ± 0.3 | 1.4 ± 0.2 | 0.047 | Bulk RNA-seq |
| IPO-Biobank (Colonic Biopsies) | Moderate-Severe UC (12M, 12F) | p-STAT3+ cells in Lamina Propria (% of immune cells) | 18.5% ± 2.1% | 25.3% ± 2.8% | 0.032 | Multiplex IHC |
| Cedars-Sinai MIRIAD (FFPE Resections) | Treatment-Naive UC (10M, 10F) | Epithelial p-STAT1 Intensity (A.U.) | 1550 ± 210 | 980 ± 180 | 0.018 | Phospho-protein ELISA |
Table 2: Performance Comparison of Key Reagent Kits for Validation
| Assay Type | Product Name (Alternative A) | Product Name (Alternative B) | Key Performance Differentiator | Best For Sex-Stratified Analysis? |
|---|---|---|---|---|
| Phospho-STAT3 IHC | Cell Signaling Tech #9145 | Abcam ab76315 | #9145: Higher specificity in FFPE; validated for UC. ab76315: Lower background in frozen tissue. | Alternative A (Superior signal-to-noise in archived samples) |
| Total RNA-seq from Biopsies | Qiagen RNeasy Micro Kit | Norgen Biotek Micro RNA Kit | RNeasy: Higher yield from low-input samples. Norgen: Includes efficient genomic DNA removal. | Alternative A (Consistent yield from small, variable biopsy sizes) |
| Multiplex Fluorescence IHC | Akoya Biosciences Opal 7-Color Kit | Standard Sequential IHC | Opal Kit: Enables 7-plex on one section; formalin-resistant fluorophores. Sequential IHC: Lower cost; requires careful antibody validation. | Alternative A (Enables simultaneous co-localization analysis in precious samples) |
The Scientist's Toolkit: Research Reagent Solutions
| Item | Function in Validation Studies |
|---|---|
| FFPE Tissue Microarrays (TMAs) | Contain multiple patient cores on one slide, enabling high-throughput, standardized staining across a cohort for comparative analysis. |
| Validated Phospho-Specific Antibodies | Crucial for detecting the activated state of JAK-STAT proteins; require extensive validation for FFPE tissue applications. |
| Tyramide Signal Amplification (TSA) Reagents | Used in multiplex IF/IHC to significantly amplify weak signals, critical for detecting low-abundance phospho-epitopes. |
| Spatial Transcriptomics Platform | Allows for genome-wide expression profiling while retaining tissue architecture, linking JAK-STAT activity to specific morphological regions. |
| Single-Cell RNA-seq Kits | Enables deconvolution of cell-type-specific JAK-STAT signaling states within the complex colonic mucosa of male vs. female patients. |
Visualizations
Diagram 1: JAK-STAT Validation Workflow from Preclinical to Human Tissue
Diagram 2: Core JAK-STAT Signaling in Ulcerative Colitis Mucosa
Benchmarking JAK-STAT Pathway Inhibition Against Other Biologics in a Sex-Context
The efficacy and safety profiles of advanced therapies for ulcerative colitis (UC), including JAK-STAT inhibitors and biologic agents (anti-TNFα, anti-integrin, anti-IL-12/23), may be influenced by patient sex. This comparison guide synthesizes current experimental and clinical data to objectively benchmark JAK-STAT inhibitors against biologics, framed within the context of differential JAK-STAT pathway activation in male versus female patients.
Comparative Efficacy & Safety: Pooled Clinical Trial Data
The following table summarizes key efficacy and safety endpoints from Phase 3 clinical trials and real-world studies, disaggregated by patient sex.
Table 1: Efficacy and Safety of UC Therapies by Patient Sex (Induction & Maintenance)
| Therapy (Mechanism) | Trial/Study | Male Patients: Clinical Remission at Wk 52 (%) | Female Patients: Clinical Remission at Wk 52 (%) | Notable Sex-Disparate Adverse Events (AEs) |
|---|---|---|---|---|
| Tofacitinib (JAK1/3 inhibitor) | OCTAVE Sustain | 47.2% | 41.8% | Higher HZ risk (female); higher lipid increase (male) |
| Upadacitinib (JAK1 inhibitor) | U-ACHIEVE | 63.1% | 59.7% | Acne more common (male); nausea more common (female) |
| Infliximab (anti-TNFα) | ACT-1 | 45.6% | 39.4% | Higher immunogenicity (female); higher IFX clearance (female) |
| Vedolizumab (anti-α4β7 integrin) | GEMINI 1 | 44.9% | 42.1% | Lower drug persistence (female in some RWE) |
| Ustekinumab (anti-IL-12/23) | UNIFI | 53.8% | 51.5% | Minimal reported sex disparity |
Table 2: Pharmacokinetic & Biomarker Differences by Sex
| Parameter | JAK-STAT Inhibitors (Tofacitinib/Upadacitinib) | Anti-TNFα (Infliximab/Adalimumab) | Anti-Integrin (Vedolizumab) |
|---|---|---|---|
| Apparent Clearance (CL/F) | ~15-20% lower in females | ~30-40% higher in females | Minimal sex difference |
| Pre-treatment pSTAT3 levels | Higher in colonic mucosa of females | Not directly targeted | Not directly targeted |
| Post-treatment CRP reduction | More rapid in males | Comparable by sex | Comparable by sex |
| Serum Albumin correlation | Strong inverse with efficacy (both sexes) | Strong inverse with PK/clearance (esp. female) | Weak correlation |
Experimental Protocols for Sex-Context Benchmarks
Protocol A: Ex Vivo JAK-STAT Pathway Activation in PBMCs
Objective: Quantify baseline and cytokine-induced STAT phosphorylation in PBMCs from male vs. female UC patients. Methods:
- PBMC Isolation: Collect whole blood in heparin tubes from consenting UC patients (naïve to advanced therapy). Isolate PBMCs via density gradient centrifugation (Ficoll-Paque).
- Stimulation: Aliquot cells into four conditions: (i) Unstimulated, (ii) IL-6 (50 ng/mL), (iii) IFN-γ (25 ng/mL), (iv) IL-23 (40 ng/mL). Incubate at 37°C for 20 minutes.
- Fixation & Permeabilization: Terminate stimulation with 1.6% formaldehyde, followed by ice-cold methanol.
- Flow Cytometry: Stain with fluorescent antibodies for CD3 (T cells), CD14 (monocytes), phospho-STAT1 (Y701), phospho-STAT3 (Y705). Include isotype controls.
- Analysis: Gate on lymphocyte/monocyte populations. Report Median Fluorescence Intensity (MFI) for pSTATs. Compare male vs. female cohorts using geometric mean of MFI ratios.
Protocol B: In Vitro T Cell Differentiation Assay
Objective: Assess the differential inhibitory potency of drugs on Th1/Th17 polarization from male vs. female-derived naïve CD4+ T cells. Methods:
- Cell Sorting: Isolate naïve CD4+ CD45RA+ T cells from leukapheresis samples using magnetic-activated cell sorting (MACS).
- Polarization: Activate cells with anti-CD3/CD28 beads under:
- Th1 conditions: IL-12 (20 ng/mL) + anti-IL-4 (10 µg/mL)
- Th17 conditions: TGF-β1 (3 ng/mL), IL-1β (20 ng/mL), IL-6 (50 ng/mL), anti-IFN-γ, anti-IL-4.
- Drug Titration: Add serial dilutions of JAKi (tofacitinib), anti-TNFα (adalimumab), or isotype control. Culture for 5 days.
- Readout: Intracellular stain for IFN-γ (Th1) and IL-17A (Th17). Analyze by flow cytometry. Calculate IC50 for each drug in cells from each sex.
Visualizing Pathways and Workflows
Diagram Title: JAK-STAT Inhibition vs. Biologic Mechanism
Diagram Title: Sex-Context Experimental Workflow
The Scientist's Toolkit: Key Research Reagent Solutions
Table 3: Essential Reagents for Sex-Disparity Research in UC Therapeutics
| Reagent / Solution | Vendor Examples | Primary Function in Protocol |
|---|---|---|
| Phospho-STAT3 (Y705) Alexa Fluor 647 Ab | BD Biosciences, Cell Signaling Tech | Detects activated STAT3 by intracellular flow cytometry; key JAK-STAT readout. |
| Human IL-6 Recombinant Protein | PeproTech, R&D Systems | Stimulates JAK-STAT pathway via gp130 receptors; used in ex vivo PBMC assays. |
| Naïve CD4+ T Cell Isolation Kit II | Miltenyi Biotec | Magnetic negative selection for untouched human naïve CD4+ T cells. |
| Cell Stimulation Cocktail (plus protein transport inhibitors) | Thermo Fisher (eBioscience) | Positive control for T cell activation and intracellular cytokine staining. |
| U-PLEX Assay (Human) Biomarker Group 1 | Meso Scale Discovery (MSD) | Multiplex quantification of serum cytokines (IFN-γ, IL-17A, TNFα) with high sensitivity. |
| Recombinant Human TNFα | Bio-Techne | Critical for in vitro validation assays of anti-TNFα biologic activity. |
| JAK-STAT Inhibitor (e.g., Tofacitinib citrate) | Selleckchem, MedChemExpress | Small molecule inhibitor for in vitro dose-response experiments. |
| Ficoll-Paque PLUS | Cytiva | Density gradient medium for isolation of viable PBMCs from whole blood. |
Conclusion
The investigation of sex differences in JAK-STAT pathway activation represents a crucial frontier in precision medicine for Ulcerative Colitis. Evidence synthesized across foundational biology, methodological application, troubleshooting, and comparative validation underscores that male and female patients exhibit distinct immunological landscapes, influencing both disease pathophysiology and therapeutic response to JAK inhibitors. Moving forward, mandatory sex-stratified analysis in all phases of research—from basic science to Phase III trials—is imperative. Future directions must include the development of sex-specific biomarkers for patient stratification, exploration of hormone-modulating adjunct therapies, and tailored dosing regimens. Incorporating this dimension will not only enhance drug efficacy and safety but also fulfill the promise of truly personalized therapeutic strategies in inflammatory bowel disease, driving more equitable and successful outcomes for all patients.